Malaka Gharib/NPR
Each week, we answer frequently asked questions about life during the coronavirus crisis. If you have a question you’d like us to consider for a future post, email us at [email protected] with the subject line: “Weekly Coronavirus Questions.” See an archive of our FAQs here.
We’ve been answering coronavirus questions from our audience for over a year, but this past week, I had some questions of my own. While on vacation with my family, I encountered four tricky COVID-19 situations. I really wanted an expert’s advice.
So I interviewed three COVID-19 specialists: Charlotte Baker, an assistant professor of epidemiology at Virginia Tech; Abraar Karan, an infectious disease doctor at Stanford University; and Jill Weatherhead, an assistant professor of adult and pediatric infectious diseases at Baylor College of Medicine. Here’s what they had to say about my concerns.
What if you’re exposed to someone who has COVID-19 — directly or one step removed?
While we were on vacation, an unvaccinated child who’d tested negative for the coronavirus a few days earlier came to an outdoor gathering. He wasn’t feeling so great. That night, he became ill and tested positive for the coronavirus.
My two adult children, who attended the gathering, were directly exposed, albeit briefly. My wife and I did not attend the event but hung out with our kids in a hotel room for a couple of hours immediately after the gathering. None of us were wearing masks.
We are all fully vaccinated. But we had so many questions! Should our kids quarantine and then get tested? And what about us? We figured we should avoid seeing our kids until their status is known … but were we at any risk of coming down with COVID-19?
All three experts said our children were at low risk of contracting COVID-19 because of their vaccine status and because the event was outdoors, where airflow does a good job dispersing pathogens. And they were only in close proximity with the little boy for a maximum of 10 minutes or so.
Yet the risk is not zero.
The experts’ recommendations: My kids should mask up when they are in public settings, indoors and outdoors, for three to five days in case they were infected and contagious. They should monitor for any potential COVID-19 symptoms such as fever, chills or sniffles. After that time period, they should get a coronavirus test. By that time, there’d be enough viral load for a test to pick up any possible infection.
The experts say it’s best to go to a health provider for a PCR test, which detects genetic material of the virus and thus provides more accurate results than the at-home antigen tests, which assess viral load.
One of my children was planning to fly home on Monday, two days after the exposure. The experts said that was OK given a) they were vaccinated and b) they’d wear a mask.
And what about my wife and me?
Karan, the doctor at Stanford, says that even if our children were infected at the gathering, the virus takes a couple of days to incubate before it can be transmitted. So we were basically in the clear. But out of an abundance of caution, we masked up in all public settings (which we do anyway because of our concern about breakthrough infections).
Our children waited three days and got tested. The results: negative! That gave my wife and me additional reassurance that we had no worries from the incident, so we could resume contact.
But what if our children were not vaccinated? Then it would have been a different story. The Centers for Disease Control and Prevention recommends an unvaccinated person — whose chances of getting infected and thus being contagious are greater than those who are vaccinated — should quarantine at home for 14 days after an exposure.
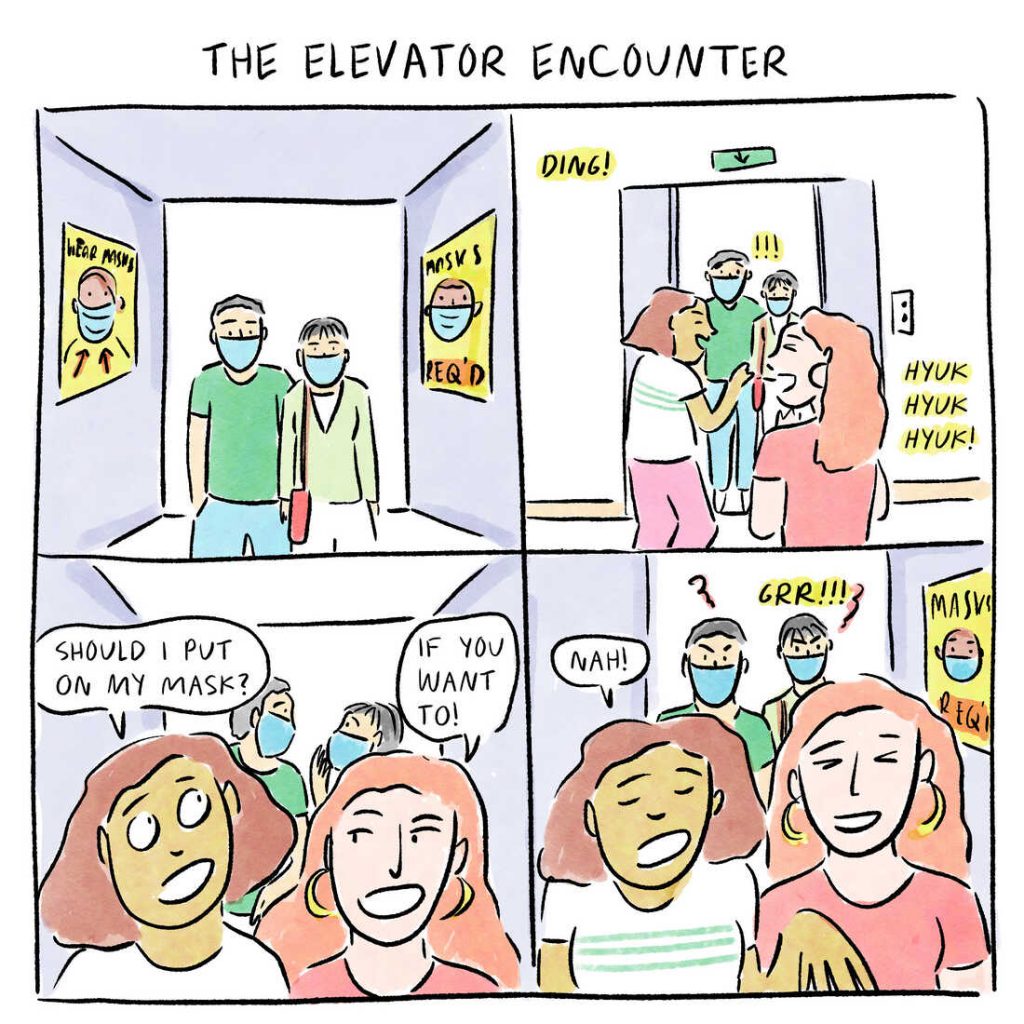
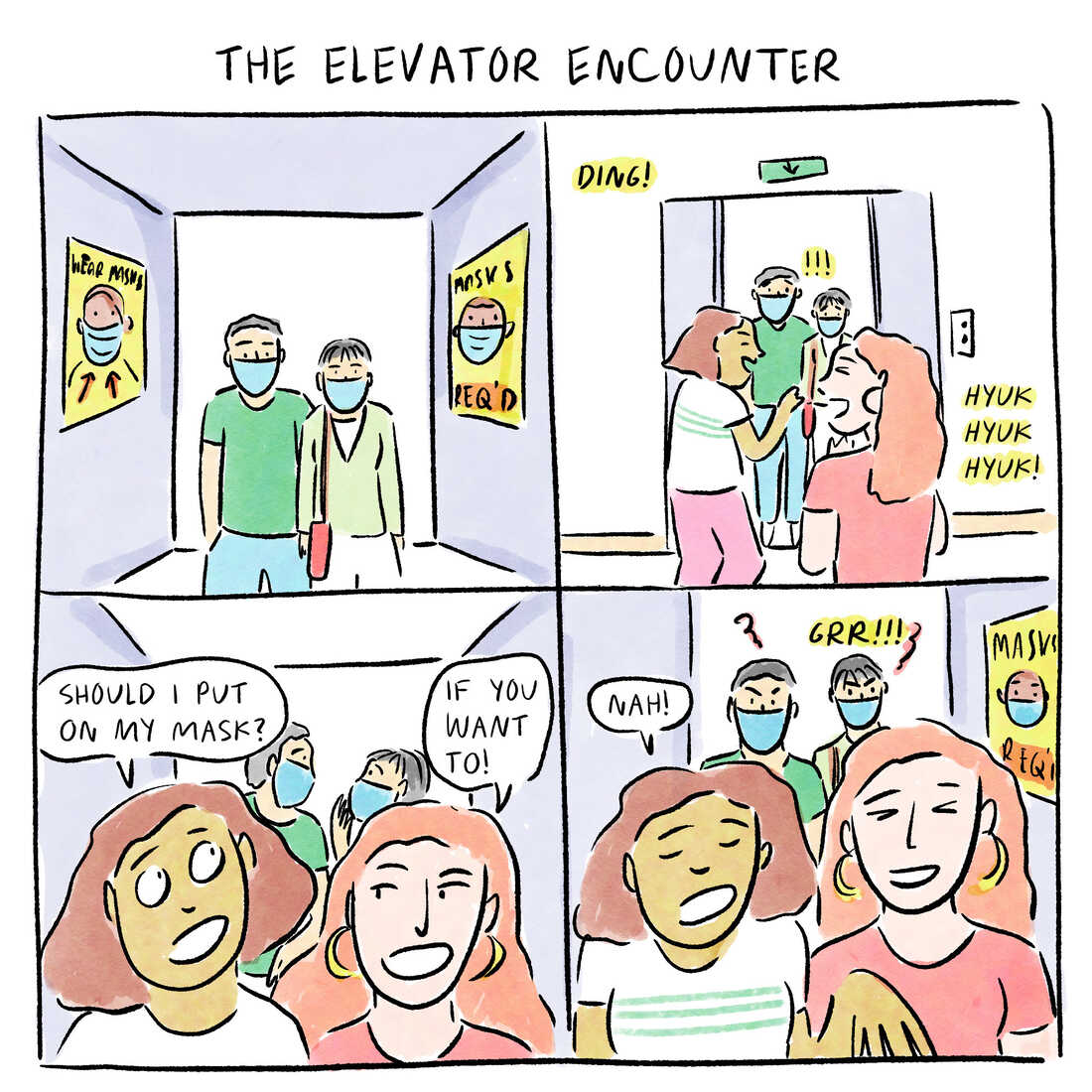
What should you say if you’re in an elevator and two maskless people enter at the next stop?
There were other moments of concern during our stay that had nothing to do with the little boy who had COVID-19. We were staying at a hotel. My wife and I got on an elevator, which had a sign on the door stating: “Guests should wear face coverings in the elevator.”
We had on masks. Two women without masks got on and eyed my mask.
“Should I put on a mask?” one asked.
“Well, if you want to, you can,” her friend replied.
Neither of them wanted to do so.
I didn’t say anything. And got off at the next elevator stop.
I wondered: Should I have spoken up?
Karan notes that in a fleeting elevator contact, an individual with a good mask (an N95 or KN95, for example, and not a thin cloth mask) would be unlikely to become either infected or spread the coronavirus.
You also have to ask yourself, he says: “Do I think saying something is going to get them to put a mask on?”
But there are other perspectives. Baker, the epidemiologist at Virginia Tech, has a medical condition that puts her at higher risk of getting infected and of severe disease. She says she would have either put in a polite request — “Please ma’am, could you put your mask on?” — or left the elevator at the next stop.
If you’re uncomfortable in an elevator for any reason – unmasked people, too crowded — “you could always get off and take the stairs,” adds Weatherhead, the assistant professor at Baylor College of Medicine.
There’s another issue to consider besides a personal concern about the odds of catching COVID-19. “This is a community-based virus,” Weatherhead says. “Unless everybody has buy-in [regarding protective measures], really nobody’s going to be safe. Everybody has to do their part.”
Which brings me to my next situation. …
If all the staff in a hotel are masked, should I mask up, too?
As I walked down the hallways of the hotel, I was struck by a noticeable mask fact. The housekeepers and other employees walking the halls were all masked. The guests by and large were not.
Now it is true that these hotel employees are in contact with a greater number of individuals in the course of their day than guests walking to their rooms.
And maybe these unmasked guests are all vaccinated.
But maybe some of the employees are not yet vaccinated. “There’s a lot of privilege in being able to get vaccinated,” Karan notes. For one thing, “you have to be able to take time off.”
And this hotel is in a state where the virus is currently surging and the vaccination rate is below 50%.
So what’s the advice? “The idea of masks is they are providing some protection for the [people who are wearing them] and protection for the guests in that hotel or restaurant,” Weatherhead says. And if you’re in an area with high rates of COVID-19, “Having everybody masking is really important — and not just for service staff.”
What do I say to someone who asks me why I’m wearing my mask?
My wife and I were dining at a restaurant with outdoor seating. At a table about 12 feet away sat two gentlemen. One of them noted that my wife and I were both wearing green.
We smiled. True!
Then he asked, “Do you really think you need to wear that mask outdoors?”
I didn’t get to answer — a restaurant staffer escorted the two men to a different part of the outdoor dining area because they were smoking in a nonsmoking zone.
So what might I have said?
Karan says first of all, it would be fine for my wife and me to be unmasked at the outdoor restaurant with no nearby diners. We’d have to take off our masks anyway once our food and drinks arrived.
But there’s also an argument for masks. He suggests I could have answered: “When you have high rates of transmission of disease with high levels of spread, it makes sense to wear a mask. It can reduce the chance you’ll get exposed to the virus or transmit it to others like kids or unvaccinated people.”
Baker notes, “If you’re going to partake in public activities – [going to] shops, restaurants, bars – you have to do a good job of being a good steward, which is being vaccinated, putting on your mask. That shows you’re a willing participant in society to help other people.”
And make sure it’s a good quality mask, she says: “I see a people with bedazzled masks and I’m like, ‘You’re putting holes in it!’ “
Then again, perhaps a case of COVID-19 is in everyone’s future. “The reality is you will be exposed to the virus,” Karan says. “Nobody is going to avoid exposure forever.” That is problematic for those at high risk of severe disease – and he says he is seeing an increase in breakthrough cases among older people and the immunocompromised that require hospitalization. But if you’re vaccinated, “you’ll never know — or may have mild symptoms so you think you just had a cold.”