Editor’s note: A year ago, the Des Moines Register began publishing “Inside COVID’s Siege,” a seven-part series that told stories of dedication, sacrifice, loss, pain and joy from inside Mary Greeley Medical Center. The Register returned in early January to document the pandemic’s ongoing toll as another surge of COVID patients taxes a weary staff.
AMES, Iowa — Last night’s grief lingers, hanging like a thick quilt over the Intensive Care Unit as nurses start their 12-hour shifts before sunrise.
The middle-aged man’s lungs had stiffened slowly since his arrival weeks earlier, coronavirus shallowing his breaths. Unvaccinated, he’d been placed on a ventilator in an eastern Iowa emergency room and shipped nearly three hours away to Mary Greeley Medical Center, site of the nearest open ICU bed.
He didn’t want to be kept alive by machines, he wrote in a living will, but loved ones couldn’t fathom withdrawing care. Keep fighting, they said. Keep fighting.
But doctors knew the battle was already lost. The virus ran through his lungs like a forest fire in a dry summer, leaving deep, painful scars scattered like charred stumps and broken branches. Nurses redoubled support, waiting for a sign of progress, hoping a little green might sprout through the blackened remains. A month on, nothing was taking root.
Family members stood over the man’s bed as the end neared, yelling accusations: You gave this to him! This is your fault!
He died as the sun set, not more than 10 minutes after nurses turned off his machines. No one in the unit had ever heard his voice, says Julie Scebold, the nurse manager. Never seen his smile.
“Which just makes the loss even more heartbreaking,” she says, looking up at her staff gathered in the break room, and down at today’s list of patients. They have a nearly full unit. Again.
Dr. Tamim Mahayni says in the current COVID wave, patients are younger, have fewer obvious risk factors and are predominately unvaccinated. (3:36)
Zach Boyden-Holmes, Des Moines Register
Mary Greeley’s ICU staff watched with angst as Iowa’s COVID cases skyrocketed this month, the curve less the usual rolling hill and more the shaft of a hockey stick. Dread crept in as the state set new positivity records. Anxiety exploded when COVID admissions ticked up, surpassing the previous highs of the hospital’s darkest waves.
And now these doctors and nurses faced a daunting reality: The pandemic’s worst might be yet to come.
Over the next month, the expected increase in severely sick COVID patients — victims of the highly contagious omicron variant — has collided with treatment shortages; an influx of admissions from now-open operating rooms and routine medical appointments; and a dangerously overburdened health care workforce, its ranks critically thinned by burnout.
There’s an “inevitability,” says Dr. Dan Fulton, the hospital’s infectious disease specialist, “that if people aren’t going to get vaccinated, they’re going to get COVID and they’re going to end up here.”
While the staff’s dedication remains, their morale has eroded. Overwhelming sadness has faded into dull numbness, a necessary callous for souls weighed down by so many traumatic losses.
Now, when patients are extubated, no commemorative song plays across the hospital, no nurses dance in the aisles. Now, discharge celebrations are muted. The newly saved leave carrying the staff’s hopes that they will become advocates fighting misinformation in their echo chambers.
Now, when there are victories, says Dr. Tamim Mahayni, the ICU’s director, they just don’t feel like victories.
Zach Boyden-Holmes/The Register
Plagued by a crisis of hope, the staff know all too well that positive cases today will bear them patients in two weeks and body bags in a month. They understand deeply that it’s here, inside the hospital, where the virus’s cruel toll on the careful is witnessed, where the price of bad decisions is paid.
So, despite overwhelming exhaustion, they steel themselves for another new peak — what they hope will be the last gasp of a six-month stretch that saw fractious families, younger, more adversarial patients, and death that feels utterly “unnecessary,” Mahayni says.
“A year ago, we had hoped the vaccine was going to bail us out of this,” he says as he prepares for morning rounds. “It didn’t even cross my mind that there would be people who didn’t want the vaccination, and it didn’t cross my mind that there would be people who so angrily didn’t want the vaccination.”
“We had a way out,” he adds, looking in on the patient in Bed 6, a case that’s the mirror image of the man they lost not 12 hours ago.
“People just didn’t take us up on it.”
Rodney Eurom, a previously healthy auto mechanic, has been on a ventilator’s maximum support for about 24 hours, and his condition isn’t improving. He’s been in the ICU’s Bed 6 for two weeks, needing more and more oxygen every day, the same tragic trajectory Mahayni has seen in patient after patient.
“At this point, if his heart were to stop and we were to do chest compressions, his chance of any meaningful recovery is incredibly low,” Mahayni tells Rodney’s daughter, Jennifer Harrison, who chokes back tears through the phone.
“At that point, we’re likely just breaking his ribs.”
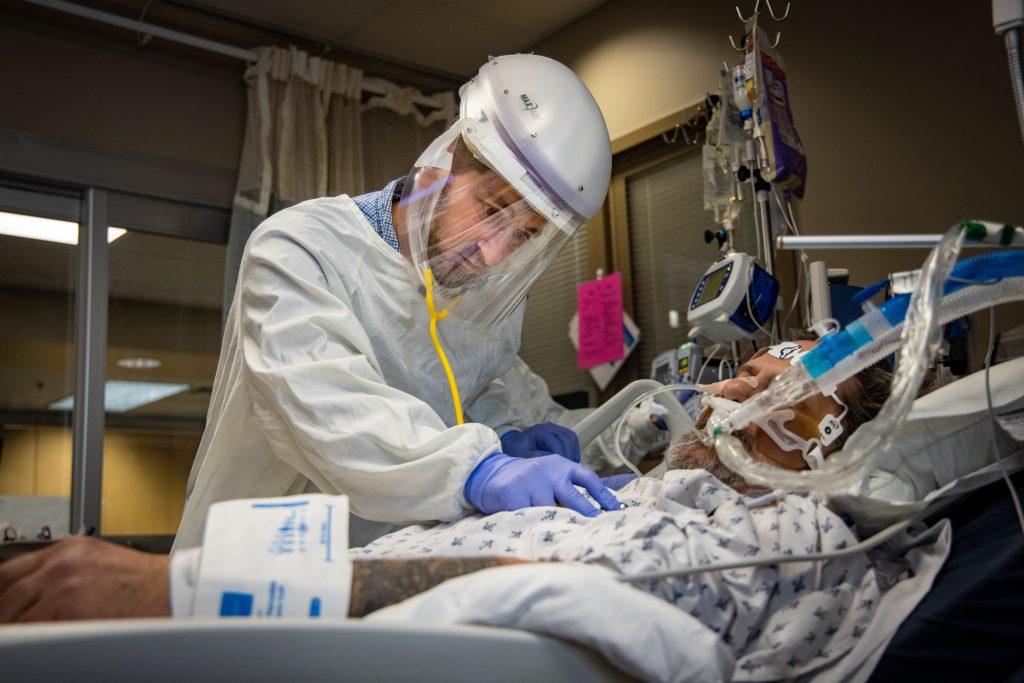
Respiratory therapist Dana Baker and nurse Abbey Malone work with COVID-19 patient Rodney Eurom in the ICU.
Respiratory therapist Dana Baker and nurse Abbey Malone work with COVID-19 patient Rodney Eurom in the ICU.
Zach Boyden-Holmes/The Register
Barely able to manage tying his robe and shuffling into old gym shoes before the ambulance arrived at his Marshalltown home, Rodney told his daughter he was weaker than wet paper. He couldn’t keep anything down, he said, the result of a bad stomach bug he’d been fighting for about 10 days.
But Jennifer noted a new shallowness in his speech, a hoarseness in his voice.
Dad, are you having trouble breathing? she asked.
Yeah, I just can’t seem to catch my breath, he replied.
Go to the hospital, Jennifer pleaded. Right now.
By the time he tested positive at admission, Rodney was already too far into COVID’s course for any of the recommended early treatments.
Hanging up with Mahayni, Jennifer buys a one-way ticket on an evening flight out of Rhode Island.
I’m on my way, she texts her dad.
I need you to know, I am on my way.
After fighting the pandemic for more than a year, the summer of 2021 tricked the ICU staff into believing the crush of COVID was abating, that the firehose onslaught was finally — finally — slowing to a trickle.
For two weeks, the ICU didn’t have a single COVID patient. No one died from the virus in May or June. The sixth floor, which had been the hospital’s COVID unit, opened half its beds to postsurgical care, returning to its prepandemic function. Carts carrying COVID-required protective gear were wheeled off the floor and into closets.
A few glorious weeks, Scebold says, when everything felt normal.
Zach Boyden-Holmes/The Register
But then came the fall. October and November brought more cases, more patients and more exposed employees. As COVID marched across the country, critical care beds became scarce; rehabilitation centers and nursing homes filled, too. Nurses called from Davenport, Sioux City, Minnesota, western Nebraska, even Waco, Texas, hoping they could find a bed for a gravely ill patient.
And, despite vaccination, 2021’s holiday season felt just as overwhelming as 2020’s, Mahayni says.
“Part of that is because it’snot grandma and grandpadying now,” Mahayni says. “It’s mom and dad.”
Patients in their 40s and 50s have been the norm in this wave, and the ICU has had a handful of 20- and 30-year-olds needing critical COVID care, too. People seem sicker, nurse Abbey Malone says, with fewer obvious risk factors and increasingly more devastating side effects, which keep them in the hospital longer.
The ICU may see more survivors, but the staff also see the ruin left behind, all the ways their patients’ lives will never be the same.
“It sounds morbid, but sometimes I feel like COVID is just finding more creative ways to hurt people,” Malone says.
For the unvaccinated, patient-provider relationships tend to start at a more adversarial point, especially if someone is sick enough to be in the ICU. Families are increasingly asking for “a la carte medicine,” Mahayni says, refusing some treatments because of misinformation, requesting others because of a headline on Facebook or a video on TikTok.
Several patients died believing their COVID diagnosis was false, that doctors were missing some sort of other weird fungal infection. Another had ivermectin — anti-parasitic tablets not approved by the FDA but touted in some alt-right circles as a miracle drug — delivered to her hospital room, a violation of Mary Greeley policy. The patient’s prescription had been written by a physician’s assistant in Wisconsin, filled by a pharmacy in Phoenix and brought to the hospital in a bundle of other mail by a friend.
Zach Boyden-Holmes/The Register
Nurses giving updates have been cussed out by patients sure that the staff’s medical care, not the virus, is what’s actually killing them. Family meetings at bedsides have become so heated security has been called. In the sixth floor COVID unit, nurses continue to play cop to patients’ visitors, reminding them to wear a mask, to gown up.
“You know these don’t work,” a family member scoffed at nurse Marjie Dyson, pointing at his mask.
“I’m sorry you feel that way,” she replied.
I’m sorry you feel that way. I’m sorry you feel that way. The phrase has become Dyson’s mechanical refrain, a kind of bulletproof vest protecting her from disinformation’s flak.
Life inside the hospital, Mahayni observes, is not immune to the divisions outside its doors.
Even if the majority of people are kind and appreciative, the bad experiences are so bad, they grate.
“Last year, I was never accused of doing things to their loved ones,” Mahayni says. “Last year, I was never accused of, ‘Why aren’t you doing this for my loved one?’”
The woman in Bed 5, a mother in her 40s, is groggy and delirious.
Orange rays, the morning’s herald, bounce off the stuffed dog and glittered drawings her kids have sent over her 47 days in the hospital. A pair of cheery speech therapists switch out the cap on her tracheotomy, a small tube placed in the windpipe when breathing help is needed long-term. Normally, the “trach” renders her mute, air bypassing vocal cords and going straight to lungs, but this cover lets her interact in short bursts.
Zach Boyden-Holmes/The Register
“Can you say hello?” one of the therapists asks.
Despite her diaphragm pumping like she’s yelling into the wind, the woman’s voice is wispy and faint, barely audible over the room’s cacophony of beeps and hums.
“Hello,” she squeaks.
A few days earlier, when the woman was coming to after surgery and before she was strong enough to speak, nurses could tell she was trying to communicate, that she wanted to say something desperately. They placed a template of pictures in front of her, made for people to point at what they might need — food, bathroom, phone — or how they might be feeling.
She wrestled with a pen, trying to write a note. But her weakness yielded only scribbles.
So she circled a trio of emotions in the corner: Lonely, worried, afraid.
As fall days grew shorter and patient counts increased, intensity inside the hospital rose slowly, like a kettle on low heat. Cases begat hospitalizations begat deaths. And as much as the staff have become experts in compartmentalization, the pain of those deaths sits just under the surface, like a cut that’s scabbed but not healed.
For Mahayni, the man in his 40s who died just before Thanksgiving is forever seared into memory. He’d received one shot of a two-dose vaccine, opting not to finish because of the side effects. A few months later, a colleague came to work sick.
The man started out on the COVID floor, then transferred to the ICU, following the tragic trajectory of needing more and more support. His teenage daughters waited in the chapel as Mahayni and the team tried to put the man on a ventilator, desperate to get his oxygen up.
But he crashed.
Zach Boyden-Holmes/The Register
In the shadow of the sanctuary’s altar, its centerpiece a stained glass dove, he told the family that their father was gone. Then he walked over to the office of his wife, also a doctor in the hospital, and cried in her arms.
The man died with 40 years of life left to live, Mahayni says.
“I look at my children and think, what is their potential? What are they going to choose to do? What kind of trouble are they going to get into? Who are they going to marry?”
“I can’t imagine not being around to see any of that,” he says, looking away. “It’s too much to think about.”
Scebold keeps a list of the COVID patients they’ve lost taped up in her office. Mahayni and her nurses still talk about them, letting stories salve the difficult memories.
There was the local firefighter whose law enforcement colleagues stood watch over his body, forming a processional as their fallen brother was carried back to his hometown. Or the patriarch on a ventilator whose unvaccinated son stood outside his room’s glass doors every day. When the end came, the son’s wife, who had to be vaccinated for work, gowned up and read a letter from him at his father’s bedside.
There were all the family members who sobbed as they told nurses they’d been fighting with their loved ones about getting vaccinated. And all the patients who changed their minds as mild cases got worse, asking for treatments they’d rejected or begging for a vaccine.
By then, the time for those interventions had long passed.
Nurses Emily Owen and Stephenie Simmons wear protective gowns, masks and face shields to check on a COVID-19 patient as the sun rises outside Mary Greeley.
Nurses Emily Owen and Stephenie Simmons wear protective gowns, masks and face shields to check on a COVID-19 patient as the sun rises outside Mary Greeley.
Zach Boyden-Holmes/The Register
The team tries to hang on to the good moments, too, the “bits of joy,” nurse Amy Olson calls them.
Like the man who asked Scebold to pray with him, trying to recite the Lord’s Prayer as an oxygen mask forced air into his lungs. His wife held vigil overnight, chanting and begging God to get her husband through. Unlike so many others, he lived.
Or the pregnant woman so sick with COVID that her baby had to be delivered by emergency cesarean section before she was put on a ventilator. The infection meant that even as the new mom slowly started to heal, she still had to be separated from her baby.
The entire hospital seemed to be following the woman’s case, Fulton says — an army reciting prayers for a happy ending.
When news that the mom and her baby would be going home made its way across the hospital, Fulton watched his colleagues lighten, as if this invisible boulder they’d all been carrying had finally lifted.
A win like that, Fulton says, revives the spirit, acting as armor against the losses they know are yet to come.
The man in Bed 2 was just passing through central Iowa on his way west when his breathing started to slow. He got dizzy, a bit light-headed. An unvaccinated semi-driver in his 50s with no significant health risks, he pulled over at a rural hospital.
For about a week, as his need for support increased, the man asked about being transferred closer to his family in the northern Midwest. But all those hospitals were full. The requests were denied.
Just after the new year, the man was put on a ventilator and life-flighted to Mary Greeley. He wasn’t showing much improvement a few days later, so Mahayni asked nurses to prone him, the difficult process of turning a patient onto his stomach in hopes of expanding his lungs.
Nurses, respiratory therapists and patient care techs gather to prone a COVID-19 patient in the ICU.
Nurses, respiratory therapists and patient care techs gather to prone a COVID-19 patient in the ICU.
Zach Boyden-Holmes/The Register
He’d prescribed the process just twice before COVID, but finds himself ordering it two or three times a week nowadays.
After 16 hours, the man needs to be turned back over, a task that requires about five nurses rolling his sheets tightly before lifting and pushing in unison. There aren’t enough free ICU hands to help, so his nurse, Treasa Throntveit, calls in for extra help. At least two people, she says.
Prepping the room, she rubs the man’s forehead.
“We need to get you turned over, don’t we, buddy,” she says.
With the move complete, a respiratory therapist resets the man’s tubes, adjusting machines and monitors now that he’s lying face up. Throntveit gently rubs a damp cloth on his cheeks. She knows the proning didn’t help, that the man’s prognosis isn’t improving.
“Don’t worry,” she repeats, tenderly wiping. “We’re here.”
The elephant in the room is vaccines. Always vaccines, Mahayni says.
“I try to think how many COVID deaths would we have seen if everybody had gotten vaccinated,” Mahayni says. “And the answer would be zero.”
“It just seems unreal,” he adds, “to think about that’s what it would have taken.”
At the beginning of the pandemic, when there was so much uncertainty and so few absolute truths, Fulton, the infectious disease doctor, became the hospital’s Mr. Rogers, a cheerleader for perseverance. It seemed he could take everything that was large and complex and scary about the virus and make it small and simple and somehow less scary.
Since the spring, he’s tried to do the same with the vaccines. He sits with patients for hours picking apart their misunderstandings. He tempers his reading of the New England Journal of Medicine with essays by the purveyors of misinformation to try to understand their logic, understand what about their arguments is so attractive.
Zach Boyden-Holmes/The Register
And he talks with employees who question vaccination, meeting them in the ICU, “where the rubber meets the road,” he says.
“Any sense that this isn’t a severe illness evaporates very quickly here.”
What he’s found under the anger and the impetuousness of many unvaccinated patients is fear, deep fear. Like the old man who broke down, revealing he’d just been so scared that getting the shot would bring his cancer back. Or the family members at the end of hope, grasping at sham treatments in a desperate attempt to stave their loved one’s suffering.
The unvaccinated are not abstract, he reminds himself. They’re real people, salt of the earth people. There’s been a failure to educate, to get them the right information in the right way — a failure he takes on his own shoulders.
“There’s this sense of sadness and regret, but there’s also this kind of existential regret,” he says, “Like, couldn’t we have gotten to him months ago to get him in the lifeboat, get him protected back then.”
“We didn’t get that done.”
Last night’s grief lingers again, that familiar quilt of angst greeting nurses starting their 12-hour shifts. As morning dawns, a new day promises more milestones of anguish and glimpses of rare joy.
In Bed 2, doctors and nurses couldn’t stabilize the truck driver. His sister drove in to be at his bedside as his ventilator was removed, holding his hand as he passed. She bagged up his few personal items, and got back in her car.
She was heading west to see her parents, she said. They’d both recently been exposed to COVID.
The mid-40s mother in Bed 5, nearly two months into her hospital stay, transfers up to the sixth floor to recuperate. After resetting wires, nurses place the stuffed dog on a shelf and tape up her kids’ glittered drawings.
She’s at the beginning of a very long journey to recovery, Fulton says.
But she’s better, a rare win for the ICU team.
Zach Boyden-Holmes/The Register
A few hours later, a middle-age man takes her place in Bed 5. He’s COVID positive, unvaccinated, and needing more and more support every day. He’s at the start of the disease’s tragic trajectory.
I didn’t know COVID could make you this sick, the man tells his nurse as she adjusts his pillow.
In Bed 6, Rodney’s room, Jennifer rubs her dad’s feet, kneading meticulously. Her days at his bedside have been a dance of a step forward, a step back.
“But we know we’re going to have a breakthrough,” she says, massaging as worship music blasts from the iPhone she’s placed on his belly.
“We’re going to have a miracle, aren’t we?” Her dad may be sedated, but she believes he can hear her, believes he can feel her presence.
On the other side of the room’s glass doors, Mahayni and his nurses wait for a sign of progress, hoping, desperately, that a little green may sprout through the blackened remains.
Courtney Crowder is the Register’s Iowa Columnist and the editor of Iowa Mourns, the Register’s collection of obituaries written to honor Iowans who have died from COVID-19. She traverses the state’s 99 counties telling Iowans’ stories. Reach her at [email protected] or 515-284-8360. Follow her on Twitter @courtneycare.
Zach Boyden-Holmes is a photographer for the Register. Follow him on Twitter @Boydenphoto.