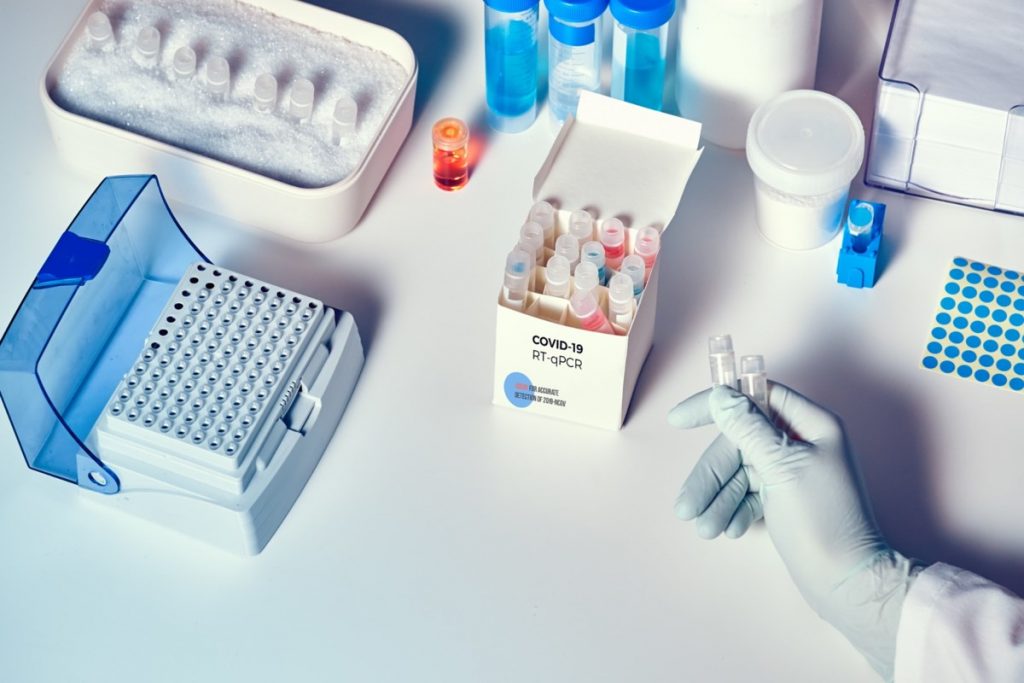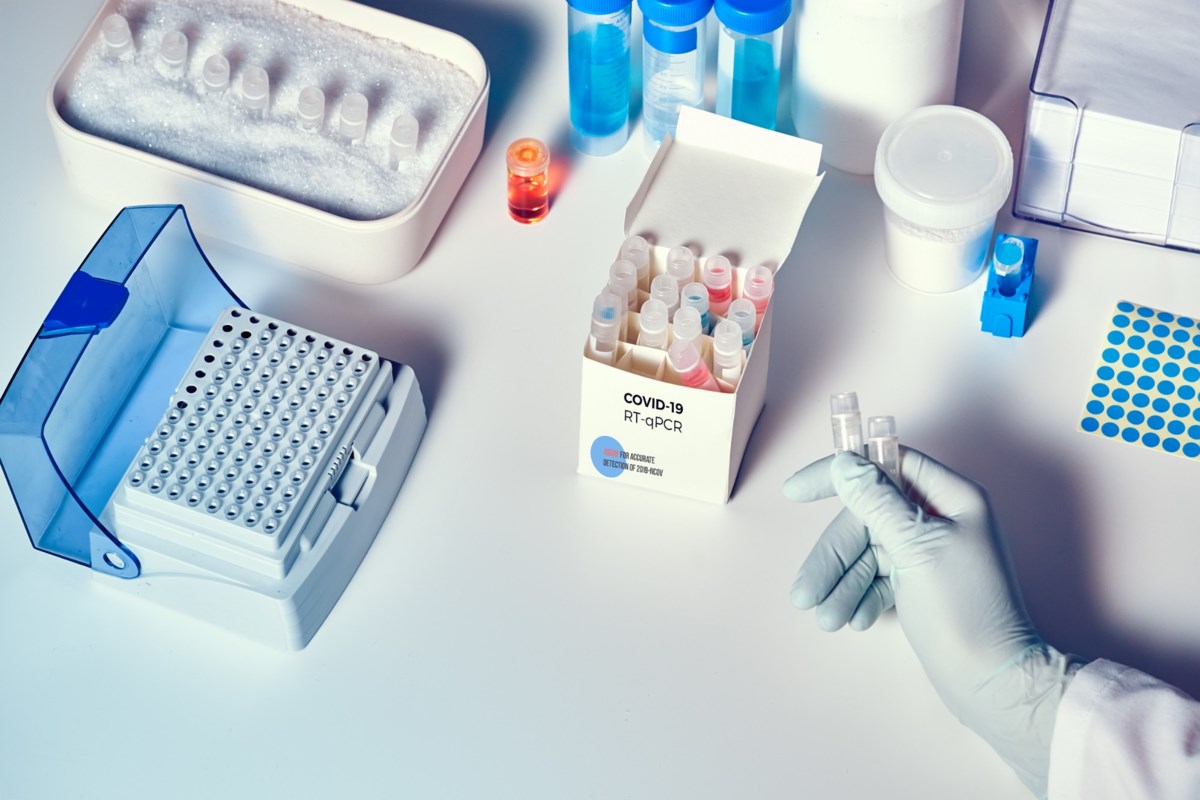
Region of Waterloo Public Health reported four new cases of the coronavirus on Wednesday morning.
Two are due to community transmission, while the other pair are tied to travel.
So far this week, there have been 12 new cases, and a total of 1,410 since March.
The number of active cases increased by three to 25, with two of those cases currently receiving treatment in hospital.
One more case has also been resolved, improving that total to 1,263.
A total of 119 local deaths have been linked to the virus, but there have been no additional deaths reported since July 17.
Meantime, an outbreak remains active at A.R. Goudie long-term care – a resident tested positive, but no more residents or staff have since it was first declared on August 3.
Here’s the provincial COVID-19 breakdown for Wednesday:
- 40,289 total cases (95 new)
- 49 people are being treated in hospital
- 36,590 resolved cases
- 2,787 deaths (one new)