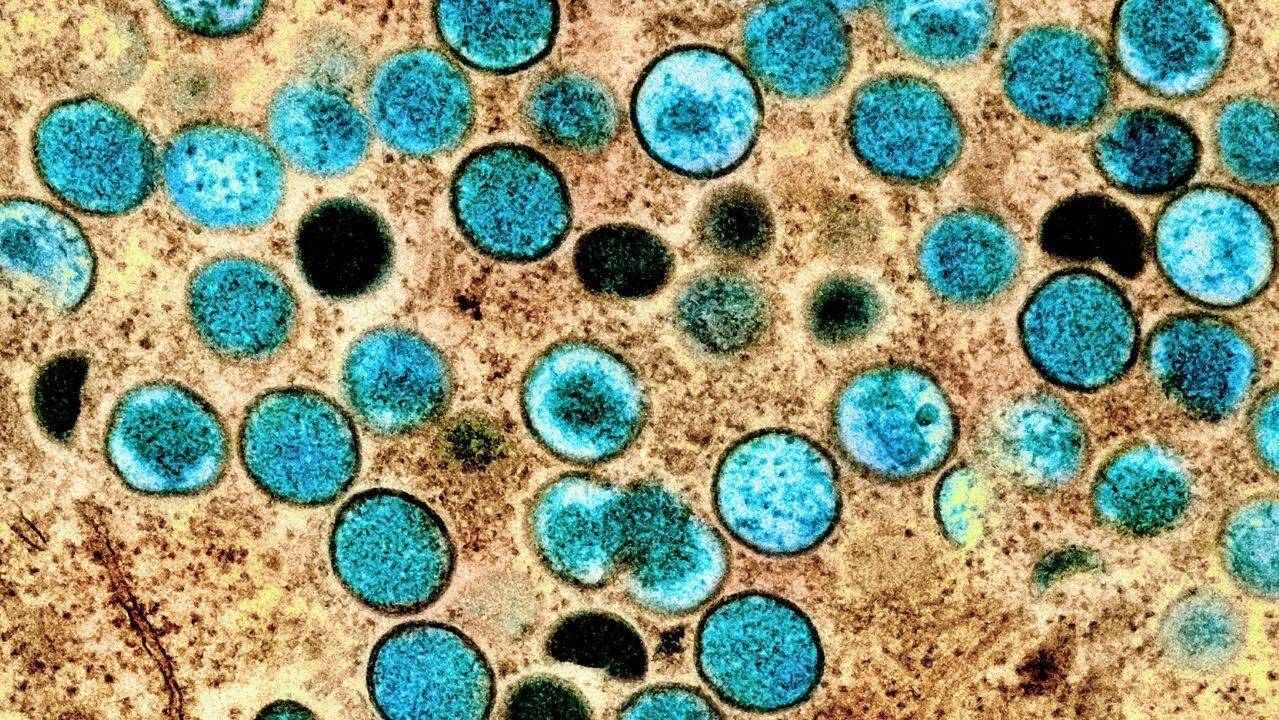
Can you catch monkeypox from a toilet seat, or by trying on clothes at a thrift store? Is the virus spreading through bodily fluids? Can you pass it to your pets?
Search for “monkeypox” on social media, and those are the kinds of questions you’ll find online.
Several months into an unprecedented outbreak of monkeypox, platforms like Instagram, Twitter and TikTok are rife with sensationalized posts about how this virus might transmit, stoking potential fears that people can catch it in their day-to-day lives, even as data overwhelmingly points to sexual contact between men as a primary driver of global transmission.
One analysis of monkeypox-related posts on Twitter, which was published in June as a letter to the editor in the Journal of Infection in Developing Countries, found more than half the posts contained misinformation or unverifiable details.
“There is a big difference between what is possible, and what is likely, and what is actually happening,” said Len Tooley, director of evaluation at the Community-Based Research Centre, a queer health policy organization, and one of the first people to catch monkeypox in Toronto.
“What we see actually happening is it is mostly gay and bi men who are getting monkeypox. Most of them are getting it sexually … so if you don’t fit into one of those two categories, you probably don’t have too much to worry about.”
While there are still key unanswered questions about the exact ways this virus spreads between hosts, data shows the bulk of infections remain among men who have sex with men — making it crucial, scientists say, to prioritize limited vaccines and supports to gay, bisexual and transgender individuals who are the highest risk of catching what’s often a painful, weekslong illness.
“We know that sexual transmission in men who have sex with men is an important mechanism of spread and is contributing significantly to the ongoing outbreak,” said physician and researcher Dr. Boghuma Titanji, an assistant professor at Emory University in Atlanta. “That being said, it is not the only method of transmission.”
So here’s what global researchers know — and don’t — about how this virus transmits.

How much does monkeypox spread through sex?
Before this year’s global outbreak, scientists typically thought the monkeypox virus, or MPXV, primarily reached humans through contact with infected animals, leading to household transmission and limited outbreaks in regions of West and Central Africa where this pathogen is endemic.
But Titanji said there were hints MPXV was spreading through sexual networks as well, with Nigerian scientists ringing alarms during a countrywide outbreak in 2017 that largely impacted sexually active young men, often causing genital lesions.
“So it is possible that monkeypox has also been spreading through sexual contact and has kind of flown under the radar, and found its way into very densely connected sexual networks that allowed it to be amplified,” said Titanji.
In Canada, the disease is mostly reported among men who have sex with men, and 99 per cent of infected individuals identify as male, with a median age of 36.
Among U.S. monkeypox cases with available data, 99 per cent also occurred in men, including 94 per cent who reported recent male-to-male sexual or close intimate contact.
As cases of monkeypox climb in Canada, there are growing concerns that the vaccine is not widely available, and time may be running out to contain the spread.
Broad European data also suggests cases remain primarily among men who have sex with men between the ages of 18 to 50. According to the latest European Centre for Disease Prevention and Control risk assessment, the likelihood of MPXV spreading further in networks of people with multiple sexual partners is “considered high,” while the chance of it spreading into the broader population is “assessed as very low.”
Understanding those transmission patterns is key to knowing where to direct limited supplies, including vaccines, said Angela Rasmussen, a virologist with the University of Saskatchewan’s Vaccine and Infectious Disease Organization.
“It makes the most sense to distribute that vaccine to the people who are at the highest risk,” she said. “People who are men who have sex with men, people who’ve had multiple partners, people who’ve had sex recently.”
So is it just spreading through skin contact? Or bodily fluids?
When it comes to transmission through sex, what’s less clear is whether it’s primarily tied to skin-to-skin contact, or if bodily fluids are also playing a major role.
“One of the unknowns is to what extent — and for how long — can this be transmitted through semen,” said Toronto-based infectious diseases specialist Dr. Isaac Bogoch.
As Public Health Ontario noted in an August evidence brief, there’s not yet clear evidence of genital secretions as a “distinct route of transmission” alongside direct, intimate contact.
Several recent case studies analyzing human semen during active infections did report finding monkeypox DNA, which has been identified in other bodily fluids as well.
Other research suggests people can carry the virus without showing any obvious symptoms, such as telltale bodily or genital lesions. One recent study conducted in France, found 13 out of 200 individuals tested positive for MPXV at the time of an anal swab performed to find other potential infections — even though they were asymptomatic.
“Whether this indicates viral shedding that can lead to transmission is unknown,” the researchers wrote.
WATCH | What it’s like to recover from monkeypox:
A Toronto resident shares his experience recovering from monkeypox, while officials and advocates say more support is needed for patients during the long weeks of isolation.
Can you catch this virus from surfaces, bedding or clothes?
Monkeypox does have a knack for lingering on contaminated items, like an infected individual’s clothes or bedding. But that doesn’t necessarily mean someone else will catch it.
In one study, investigators found live virus 15 days after a patient’s home was left unoccupied, the U.S. Centers for Disease Control and Prevention noted in mid-July.
Studies also show that other closely related viruses can survive in an environment similar to a household for weeks or months, the CDC statement continued, with porous objects, like bedding and clothing, potentially harbouring live virus for longer periods than non-porous surfaces, like glass or metal.
So, theoretically, this virus can be passed on by touching various objects, or through close, non-sexual contact.
There are concrete examples of household transmission to children and possibly pets, including one case study in France where two men who caught MPXV may have passed it to their dog, who slept in their bed.
The World Health Organization says it’s very important to isolate pets from a person in the household with the disease, to avoid spread. A dog in Paris is believed to be the first case of human-to-dog transmission of monkeypox.
But if this virus was easily spread through surface-based transmission, “we would have seen a much larger outbreak ages ago,” said Bogoch.
“I think it’s completely overblown that we should be concerned about touching an inanimate object, like a doorknob going into a place, or a scooter, or washing every item that we get from the grocery store,” he said. “I think that’s obviously premature.”
Dr. Zain Chagla, an infectious diseases specialist with McMaster University in Hamilton, agreed global data on cases during this monkeypox outbreak show infections typically aren’t just “showing up out of the blue.”
“And the few that are, are not really leading to sustained transmission,” he said.
Still, Chagla said there’s merit to taking certain precautions, primarily within health-care settings and households where a family member has an active infection.
If someone in a home has monkeypox, the CDC suggests cleaning and disinfecting the entire space, and putting all contaminated clothes and linens in the laundry — and if the person doing that job isn’t the one infected, they should wear, at a minimum, disposable medical gloves and a respirator or a well-fitting mask.
What about transmission through the air?
Like lots of other common viruses, including those that cause influenza and COVID-19, MPXV can spread through the air and infect other people — though many scientists don’t see evidence yet that it’s a major transmission route.
“You can still get transmission through droplets and aerosols,” said Titanji, referring to larger and smaller sizes of particles that people can breathe out or inhale.
“But the last two modes of transmission that I’ve just listed appear to be less frequent than the predominant mode of sexual transmission.”
The World Health Organization maintains that transmission through respiratory particles “usually requires prolonged face-to-face contact,” which puts health workers, household members and other close contacts of active cases at a greater risk of getting infected.
“If people were getting monkeypox … by inhaling it and breathing it in, then we would see a lot of people who are not men who have sex with men contracting monkeypox,” said Rasmussen.
As for misinformation circulating online, implying the general public can easily catch this virus, Tooley said some of it may come from a place of stigma or simply fear.
“I hope all those people who are afraid of getting monkeypox are advocating for services for those who do get monkeypox,” he said.
“Because if it does continue spreading into other populations, we want to make sure the health-care system is prepared.”