It all started with a stomach bug.
That’s what Cheryl-Anne Labrador-Summers thought, anyway. It was October 2020, not long after she’d moved to the tranquil lakeside Ontario community of Georgina, and instead of relaxing with her family like she’d planned, the mother of three was struggling to figure out why she kept experiencing strange, unexplained stomach cramps.
Labrador-Summers tried to visit her family physician, but the office was shuttered because of the COVID-19 pandemic. So she searched for another clinic — only to be offered a phone appointment rather than an in-person assessment. She wound up being told that her grumbling digestive system was likely caused by a mild gastrointestinal illness.
By January, the 58-year-old had a distended stomach, looking — in her own words — “about nine months pregnant.” Again, she reached out to a physician, went for some tests, then headed to the nearest emergency department.
After finally seeing a doctor face to face for the first time in months, she learned the real cause of her discomfort: an intestinal blockage caused by cancer.
“It ended up being a nine-centimetre tumour, and it had completely blocked off my lower bowel,” she said.
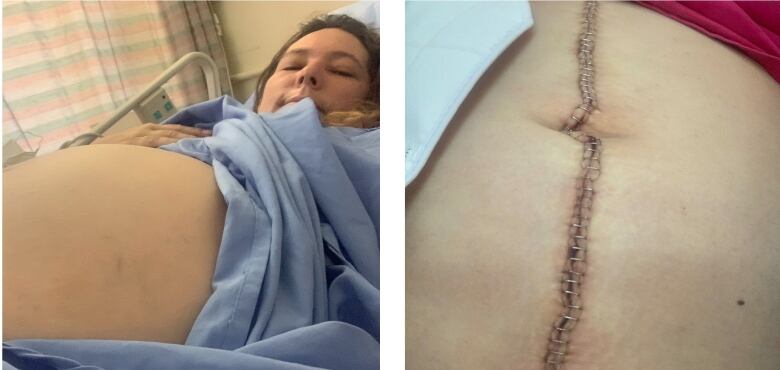
An emergency surgery left Labrador-Summers with 55 staples along her torso and a months-long recovery before she could begin oral chemotherapy. Her question now is unanswerable but painful to consider: Could that ordeal have been prevented, or at least minimized, by an earlier diagnosis?
“Had I maybe been able to see the doctors earlier, I would not be in Stage 3,” she said. “I might have been a Stage 2.”
951,000 fewer cancer screenings in Ontario
More Canadians could experience late-stage cancer diagnoses in the years ahead, medical experts warn, forecasting a looming crisis tied to the ongoing COVID-19 pandemic.
“We expect to see more advanced stages of presentation over the next couple of years, as well as impacts on cancer treatments,” said oncologist Dr. Timothy Hanna, a clinician scientist at the Cancer Research Institute at Queen’s University in Kingston, Ont.
“We know that time is of the essence for people with cancer. And when people are waiting for a diagnosis or for treatment, this has been associated with increased risks of advanced stage and worse survival.”
One review of Ontario’s breast, lung, colon, and cervical cancer screening programs showed that in 2020 there were 41 per cent — or more than 951,000 — fewer screening tests conducted compared with the year before.
Screening volumes rebounded after May 2020, but were still 20 per cent lower compared to pre-pandemic levels.
WATCH | Late-stage cancer being diagnosed in Canadian ERs:
Hospital emergency rooms are seeing a wave of patients being diagnosed with late-stage cancer after the COVID-19 pandemic forced many doctors’ offices to close or pivot to virtual appointments, leading to fewer cancer screenings.
That drop in screenings translates into fewer invasive cancer diagnoses, including roughly 1,400 to 1,500 fewer breast cancers, wrote Dr. Anna N. Wilkinson, an assistant professor in the department of family medicine at the University of Ottawa, in a May commentary piece for the journal Canadian Family Physician.
“The impact of COVID-19 on cancer is far-reaching: screening backlogs, delayed workup of symptomatic patients and abnormal screening results, and delays in cancer treatment and research, all exacerbated by patient apprehension to be seen in person,” she wrote.
“It is clear that there is not only a lost cohort of screened patients but also a subset of missed cancer diagnoses due to delays in patient presentation and assessment,” leading to those cancers being diagnosed at a more advanced stage.
Tough accessing care in a ‘timely way’
The slowdown in colonoscopies may already be leading to more serious cases of colorectal cancer in Ontario, for instance, suggests a paper published in the Journal of the Canadian Association of Gastroenterology.
“Patients who were treated after the COVID-19 pandemic began were significantly more likely to present emergently to hospital. This means that they were more likely to present with bowel perforation, or severe bowel obstruction, requiring immediate life-saving surgery,” said the study’s lead author, Dr. Catherine Forse, in a call with CBC News.
“In addition, we found that patients were more likely to have large tumours.”

In some cases — like Labrador-Summers’s situation — Canadians learned alarming news about their health in hospital emergency departments after struggling to receive in-patient care through other avenues.
Shuttered family physician offices, a shift to telemedicine, and some patients’ fears surrounding COVID-19 may all have played a role.
“It became harder for patients to access care and to access it in a timely way,” Hanna said.
“At the same time, there were real risks — and there are real risks for leaving home to go anywhere, particularly to go to an outpatient clinic or a hospital in order to get checked out.”
Dr. Lisa Salamon, an emergency physician with the Scarborough Health Network in Toronto, said she’s now diagnosing more patients with serious cancers, including several just in the last few months.
“So previously, it may have been localized or something small, but now we’re actually seeing metastatic cancer that we’re diagnosing,” she explained.
Lessons for future pandemics
Health policy expert Laura Greer is dealing with Stage four, metastatic breast cancer herself after waiting more than five months for a routine mammogram she was initially due for in the spring of 2021 — a precautionary measure given that her mother had breast cancer as well.
Unlike an early-stage diagnosis, Greer’s cancer is only treatable, not curable.
“It was an example of what happens when you don’t have the regular screening, or those wellness visits,” said the Toronto resident and mother of two.
“I most likely would have had earlier-stage cancer if it had been sooner.”

Pausing access to care and screenings for other health conditions can have dire impacts on patients, according to Greer, offering lessons for how policy-makers tackle future pandemics.
“We need to make sure that we’ve got enough capacity in our health system to be able to flex, and that’s what we really didn’t have going into this,” she said.
For Labrador-Summers, it’s hard to forget the moment her life changed while she was alone in an emergency department, learning a terrifying diagnosis from a physician she’d just met. Her mind raced with questions about the future and concerns for her family.

“My older son had just told us they were expecting a child, and I just wanted to be there for them. And I didn’t know what next steps were. And we had lost my mom to cancer a few years back — to us, cancer was always terminal,” she recalled.
“So again, I’m alone, trying to process all of this.”
A screening following Labrador-Summers’ surgery and chemotherapy treatment wound up finding more cancer.
“It’s now life-threatening,” she said.
















