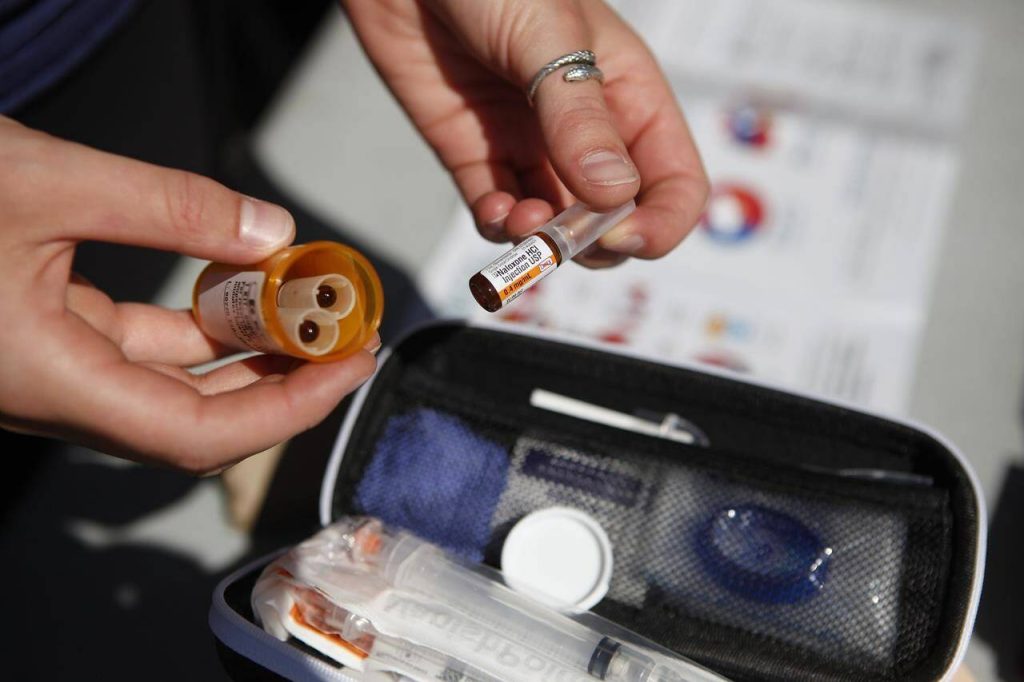
Take-home naloxone kits across Canada should contain both versions of the opioid overdose-reversing drug — a nasal spray and an injectable that goes into a muscle — says a panel of experts that includes people who use drugs.
The new guidance, led by the BC Centre for Disease Control, aims to standardize take-home naloxone kits that are distributed through various sites, including pharmacies, community groups and emergency departments, to anyone who could respond to an overdose.
Those who have used naloxone to save lives say having the nasal spray at hand could ensure a faster response because some people may be uncomfortable with needles.
Authors of the guidance, published recently in the Canadian Medical Association Journal, strongly recommend federal, provincial and territorial programs be adapted so people have a choice of methods when a fast response is needed after someone has overdosed on an illicit substance.
First responders also carry naloxone, which blocks the effects of opioids such as fentanyl, heroin, morphine and oxycodone. The medication will not work on someone who has overdosed on stimulants including cocaine, MDMA (ecstasy) and Ritalin, but will not cause harm either.
The vast majority of kits that are distributed for free across the country include injectable naloxone in ampoules or vials along with syringes, gloves, an alcohol swab and a “barrier shield”to place on someone’s face before they’re given mouth-to-mouth resuscitation. An overdose can be temporarily reversed in about three to five minutes but responders should call 911 first in case the person stops breathing again.
Three one-milligram ampoules of naloxone, also known as Narcan, are in the kits distributed in B.C., where life-saving training is provided at various sites through the BCCDC.
Dr. Jane Buxton, an epidemiologist and a senior author of the guidance, said take-home naloxone programs differ among provinces and territories, with some collecting data on distribution from pharmacies while others rely on organizations that may not be providing complete information.
“The intranasal (formulation) is available in some provinces to anybody and in others it’s more limited,” said Buxton, who recently retired as the medical lead for harm reduction at the BCCDC.
“In B.C., we don’t have the intranasal (formulation) as available as it is in Ontario.”
Naloxone nasal spray comes in a device with two prongs that fit into each nostril to administer the medication to someone who has overdosed.
It is available at no cost through a federal program to First Nations and Inuit when prescribed or recommended by a pharmacist. But, as the authors note, the high cost for provinces and territories is generally the biggest hurdle in accessing that formulation, and it varies across the country.
Ontario and Quebec offer free nasal spray naloxone at pharmacies that carry it, or through locations such as needle exchange programs, shelters and public health units.
At one pharmacy in Vancouver, about a 10-minute walk from theDowntown Eastside, the intranasal naloxone costs $75, but it is not stocked and must be ordered. Unlike the injectable version, other supplies are not included.
Buxton said having both formulations of naloxone in every kit would be ideal because someone who is not accustomed to needles could feel more confident using the nasal spray while others may prefer the intramuscular version.
“What we heard from people with lived experience is that many feel that the injectable (formulation) can be titrated better,” Buxton said.
That prevents withdrawal symptoms brought on by too much naloxone, which wears off within an hour.
“It may mean people immediately start searching for substances to get rid of that withdrawal.”
About 80 per cent of people who carry a naloxone kit use opioids themselves and may administer the medication to someone who overdoses on a toxic illicit substance, said Buxton, noting people are encouraged to not use drugs alone.
“We know we’ve had at least 150,000 overdose reversals but that’s a vast underestimate because people don’t always report,” she said.
In B.C., each intramuscular naloxone kit comes in a hard black case with a silver cross and a belt hook. Besides items such as three retractable syringes, it includes a form with a dozen questions regarding when and where the overdose occurred. But many responders may not email or fax it to the BCCDC as requested so the true number of reversed overdoses is not being counted.
The new guidance, which included input from experts across Canada, as well as the United Kingdom and Australia, also calls for responders to prioritize rescue breaths, or mouth-to-mouth resuscitation, to get oxygen into a person’s blood over massaging their heart.
“It’s part of the training in B.C., but it isn’t necessarily consistent throughout the country,” Buxton said. “Interestingly, there’s not a lot of evidence in the literature. And that’s why it was so important for us to have the insights from people who have been administering take-home naloxone, who have done thousands and thousands of reversals.”
More than 1.9 million naloxone kits have been distributed in B.C. since 2015 through 2,200 locations, according to the BCCDC, which started the country’s longest-running provincewide take-home naloxone program in 2012. A community group called Streetworks began Canada’s first naloxone program in Edmonton in 2005, based on a Chicago model, which also helped inform B.C.’s effort.
More than 37,000 people in Canada have died of a toxic drug overdose since 2016, prompting some jurisdictions to introduce safer alternatives, though Buxton said greater access to such programs is crucial as part of a comprehensive response to the overdose crisis.
In B.C., 1,455 people fatally overdosed between January and July this year, a record number of deaths in that time period since overdose deaths started climbing rapidly in 2016, when the province declared an ongoing public health emergency.
Cheryl Guardiero, a retired nurse, said she injected her son, Brett Colton Mercer, with naloxone 10 separate timesbefore he fatally overdosed alone in 2017 at age 29.
She agreed with the guidance, saying many people would be too anxious to load a syringe with naloxone from an ampoule while trying to help an extremely drowsy or unconscious person.
“If you’re rushing with adrenalin and you’re trying to clip that little glass thing apart and draw (the naloxone) up, that takes a few seconds. But for somebody that’s not used to that, it’s pretty traumatizing whereas if it’s just the nasal spray, they can just pop it up their nostrils and spray it.”
Guardiero, who recently moved from Nanaimo, B.C., to the Alberta hamlet of Wabamun, walked the streets of Vancouver’s Downtown Eastside with naloxone kits after her son died. She said shereversed four overdoses.
“Reversing overdoses down there is a different world. You go from one to the other to the other,” said Guardiero, a member of the advocacy group Moms Stop the Harm.
Marliss Taylor, program manager for Edmonton’s Streetworks harm reduction program, said the cost of a naloxonedose shipped from Chicago back in 2005 was 25 cents.
Now, a hard-shell kit with three doses of the drug and supplies costs about $30, though it’s distributed for free, and the intranasal formulation, uncommon in Alberta, sells for about $100, she said.
While the intramuscular injection kits offer more precise dosing, Taylor said including the nasal spray would prevent responders from panicking while they’re trying to inject a needle into someone’s arm or thigh, especially without adequate training.