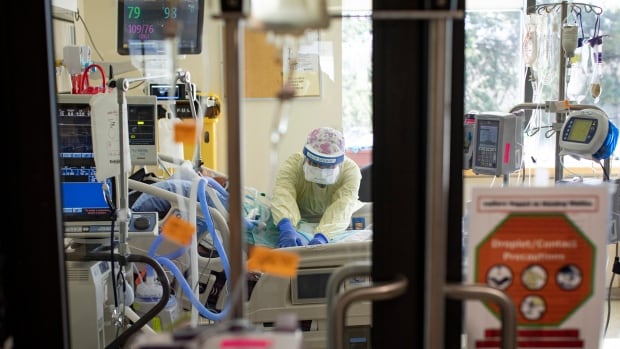
Health-care staff in B.C.’s Interior are being overwhelmed by the twin emergencies of persistent wildfires and rising COVID-19 cases, and some of them are leaving their jobs because of it.
Multiple nurses and doctors who spoke to CBC News said roughly two-thirds of emergency room nurses at Royal Inland Hospital in Kamloops had left their job in recent months due to stress and burnout.
“I would genuinely say that the situation is dire on a daily basis,” said one emergency room nurse whom CBC News agreed not to identify. “There are currently about 24 empty positions in our emergency department. I know several nurses who are considering leaving the profession or quitting nursing because it’s not worth their mental health.”
The nurse said they personally feel they are “in over my head” and constantly worry they are going to cost a patient’s life because the workload is too much to handle.
“If a fourth wave [of COVID-19] does hit and hits hard, we would not be able to accommodate that.”
Staff from other parts of B.C. asked to help
Meanwhile, two internal memos viewed by CBC News confirm other hospitals in the region are over capacity and in need of additional help, even asking people from other parts of the province to volunteer to come help.
The first, which was sent out by Interior Health on July 13, indicated the Vernon Jubilee Hospital had declared “virtual code orange” with the 196-bed facility counting 236 patients — or 120 per cent capacity — as the wildfire risk in the region increased. Code orange in B.C. means “disaster.”
The second, which has been circulated on social media, was distributed to health-care staff on Vancouver Island on Aug. 18. It asked health-care providers willing to be deployed to Interior Health to sign up with the province’s Emergency Health Provider Registry.
That registry was created during the wildfire season of 2017 to make sure staff can be deployed to health regions in need of help during emergencies.
BREAKING: Restrictions introduced in the Central Okanagan earlier this summer have been expanded to the rest of B.C.’s Interior in response to rising cases of COVID-19 throughout the region. <a href=”https://t.co/7ad0lyzfKK”>https://t.co/7ad0lyzfKK</a>
—@cbcnewsbc
On Friday, Provincial Health Officer Dr. Bonnie Henry acknowledged the stresses being felt in the Interior “as we are dealing with the displacements of peoples across the Interior Health region due to the ongoing wildfire situation,” adding, “It has strained resources in a number of communities,” including Nelson, Vernon and Kamloops.
However, she said she would not call the situation “dire.”
B.C. Health Minister Adrian Dix said asking staff to volunteer to be deployed to other health regions reflects an “extremely serious” wildfire situation in B.C., as patients and people living in long-term care in communities under evacuation alert are moved around the province, putting additional strain on staff.
“What we’re seeing in some hospitals is real pressure,” he said. “It’s something we do on a regular basis, which is to seek people to support the regions.”
Royal Inland Hospital at breaking point: doctors
However, Scott Duvall who represents the Thompson/North Okanagan region for the B.C. Nurses’ Union, said the problems in Kamloops go beyond a short-term emergency or routine staffing shortages.
Instead, he said, it’s a systemic failure that is impacting Royal Inland Hospital’s ability to recruit and retain new employees.
“I recently spoke with one of our recent new [nursing] grads from Thompson Rivers University,” he said. “She said that a large percentage of those that graduated with her are choosing not to go to Royal Inland because of their experience there [as students].”
Emergency room doctor Henk Van Zyl said the staffing shortages he’s been observing at Royal Inland are unsustainable, particularly for nurses who often bear the brunt of the extra work.
“We’ve had nurses leave their shifts crying. We’ve had nurses feeling that they can’t tolerate it anymore. They’re feeling that their job is at risk because they can’t provide good medical care,” he said. “When people lose faith that [this problem] is going to be resolved … then it becomes even more difficult to recruit new nurses, because who’s going to come when you know that the working environment isn’t conducive to a good lifestyle?”
If a fourth wave [of COVID-19] does hit and hits hard, we would not be able to accommodate that– Emergency room nurse at Royal Inland Hospital in Kamloops
Roger Parsonage, interim vice-president of clinical operations for Interior Health North, said recruitment is the health authority’s No. 1 focus as a streamlined hiring process is rolled out to attract new employees to the region.
In the meantime, though, emergency room physician Dr. Keith Hutchison warns the situation at Royal Inland Hospital is the worst he’s seen in his 32 years there. The repercussions of this summer could be felt for years to come, he said.
“We’re losing 25 to 30 per cent of our emergency nurses,” he said. “That’s huge.”