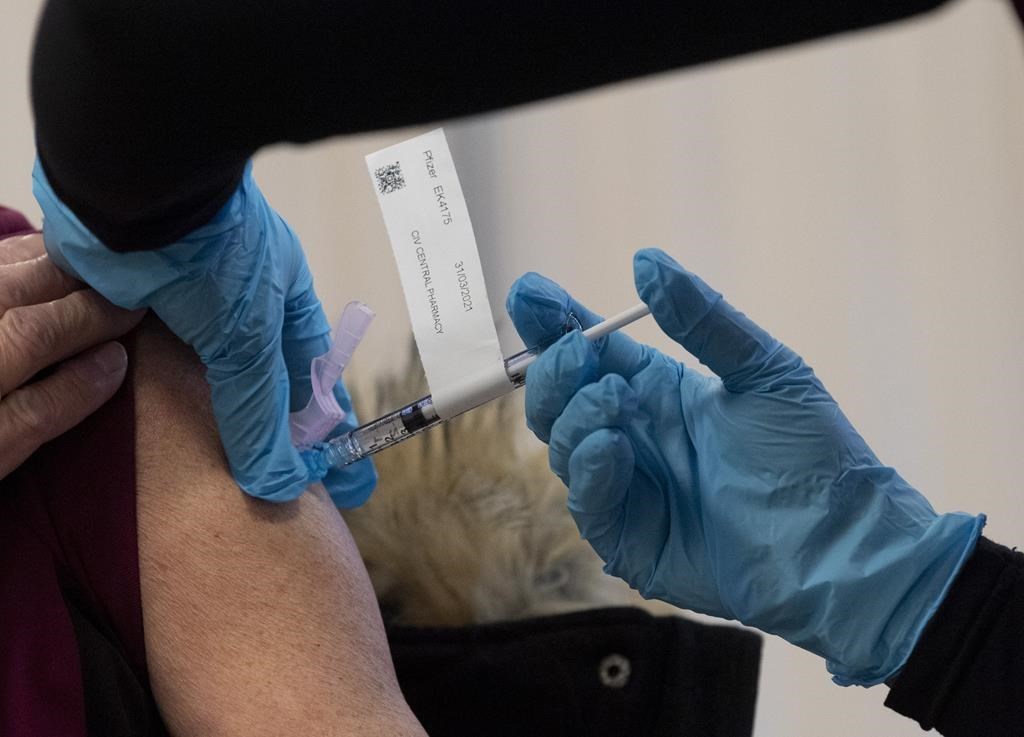
TORONTO — Family doctors are awaiting clear details of Ontario’s plan to ramp up their involvement in the COVID-19 vaccination effort.
Provincial officials said this week that they hope to include more family care practitioners in the immunization campaign in an effort to reach residents still without first doses and slowly shift away from mass clinics.
Dr. Liz Muggah, president of the Ontario College of Family Physicians, said her professional group only heard about that plan when it was publicly announced on Thursday. She said the college welcomed the news and wants to see a clear plan from the government soon.
“Our question would be, which is what we said in the beginning, what’s the plan,” Muggah said in an interview. “Let’s lay this out so that we know what’s coming, and when, and can get ready.”
The Ottawa-based physician has been among the select family doctors able to offer COVID-19 vaccines in office. Government figures note that 700 primary care sites have been administering the shots, far fewer than the thousands of pharmacies and other clinics Ontarians have had access to.
A spokeswoman for Health Minister Christine Elliott said primary care has played a critical role in Ontario’s vaccine rollout so far, adding public health units can now request more vaccine supply for primary care settings. She also said the health units have allocated vaccine to different clinic types based on local needs.
“Recognizing the vital role that primary care settings play in a patient’s health care journey, we are working with our primary care partners to take on additional vaccination capacity as Ontario’s vaccine rollout continues, allowing us to reach even more Ontarians,” Alexandra Hilkene said in a statement.
Muggah’s college and other professional doctors’ groups have been pushing for more involvement in the vaccine rollout since it began, arguing their personal relationships with patients can help reach those who are hesitant about the process or unsure how to make appointments.
Now that Ontario’s first-dose adult vaccination rate has hovered at just under 80 per cent for several weeks, the province has also started to cite the patient-doctor relationship as a powerful tool to reach the holdouts.
Ontario hasn’t set a target for how many doctors it hopes to have administering the shots, or a timeline for their involvement. Solicitor General Sylvia Jones said this week she envisions eventually having COVID-19 shots largely handled in doctors’ offices and pharmacies, much like annual flu shots.
The Ontario Medical Association, another group representing doctors in the province, said this week that it’s working with the government “to ensure that family physicians and pediatricians continue to be as involved as much as possible in the vaccine rollout,” including a push for more mRNA shots to be administered from doctors’ offices.
Informal polling by the Ontario College of Family Physicians has indicated at least 75 per cent of members want to be vaccinating against COVID-19, Muggah said. Many doctors are working in mass vaccine clinics and in other venues, but they contend they can do more to help with in-office vaccinations.
“My sense is definitely that there is a huge untapped potential in family medicine that we haven’t taken advantage of,” she said.
Doctors are already skilled in vaccinations, though Muggah said the process would involve some preparation like training on the provincial vaccine registry, implementing infection control measures and planning clinics for patients.
“All of those things are absolutely doable, so I think the main issue really is going to be getting a supply to us,” she said.
The province’s gradual shift in vaccine strategy will be welcomed by the many physicians who have been frustrated and saddened by their lack of involvement so far, she added.
Dr. Alain-Remi Lajeunesse is in the process of trying to secure COVID-19 vaccines for his Ottawa office.
About 80 per cent of his patients are now vaccinated against the virus, but Lajeunesse said he wants to be able to offer shots on the spot when he meets with patients, some of whom are convinced in one-on-one meetings to get vaccinated, but don’t follow through after they leave.
“That opportunity to vaccinate them was kind of missed,” the family doctor said. “Having that vaccine in our fridge so that we can do the counseling, they agree, and then we do the vaccine, that would be the ideal situation, so that’s what we’re trying to work towards.”
Lajeunesse said he’s been frustrated at having to wait on the sidelines throughout much of the immunization drive.
“It would be nice to have the government say overtly, ‘we want you as partners,'” Lajeunesse said. “It’s better late than never.”
This report by The Canadian Press was first published July 10, 2021.
Holly McKenzie-Sutter, The Canadian Press