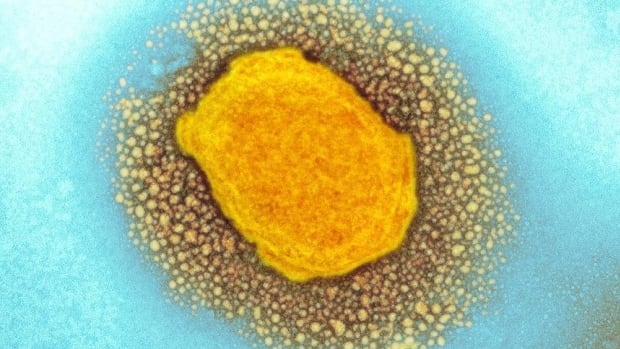
Ottawa Public Health (OPH) is planning vaccine clinics for monkeypox and has begun offering shots to residents who are “highest risk.”
Dr. Vera Etches, Ottawa’s medical officer of health, said the province provided roughly 100 doses over the weekend, which was enough to meet the immediate demand.
However, during Monday’s board of health meeting Etches said she expects interest in getting the vaccine could rise as more people learn it’s available. That’s where the clinics, which have also been held in Toronto and Montreal, would come in.
“In addition to access through our sexual health centre, we’re also planning additional clinics with partners who can best connect with communities at higher risk,” Etches said.
Public health reported the first positive case of monkeypox in Ottawa on June 10.
That person has since recovered and OPH followed up with close contacts about post-exposure vaccination, Etches said. The risk to the general public remains “very low,” she added.
Following guidance from the Ministry of Health, OPH administered the Imvamune vaccine to high-risk contacts of the confirmed case.
A Public Health Ontario summary about monkeypox states that as of June 16 one confirmed and two suspected cases of the infectious disease have been reported in Ottawa. Thirty confirmed cases have been recorded across the province.
Deep, ‘painful’ pustules
Virologist Earl Brown said monkeypox comes with a key feature — large lesions that usually start on the head and hands but can spread to other parts of the body.
“They are very uncomfortable apparently and painful,” the University of Ottawa professor emeritus explained.
“They’ve very deep pustules, they’re right into your skin and they’re little volcanoes since they’re full of clear fluid.”
We will begin offering vaccination this weekend to the highest priority individuals based on the latest provincial eligibility criteria. Those who are eligible will be contacted directly. (5/7)
—@OttawaHealth
Those sores dry and then drop off “loaded with virus,” Brown said. That’s one way the virus can spread, but the infection can pass through close contact as well as exposed skin, the respiratory tract or mucous membranes around a person’s eyes, mouth and nose.
The rare disease comes from the same family of viruses that cause smallpox, which the World Health Organization declared eradicated in 1980, but it’s “much milder,” said Brown.
Information session Thursday
Infectious disease specialists say the LGBTQ community, particularly men who have sex with men, are at disproportionate risk of infection in this outbreak. Health-care workers or lab workers who work directly with orthopoxviruses could also be at risk.
The AIDS Committee of Ottawa is set to host an information session about monkeypox on Thursday where Dr. Paul MacPherson will be on hand to answer questions from 6 p.m. to 8 p.m.
Cory Wong, manager of support services for the committee, said there’s a “sense of urgency” among those who use its services and he’s already fielded a lot of questions about when the vaccine will be available.
“It’s very relevant to people who we work with, including men who have sex with men, racialized community members and people who live with HIV with compromised immune systems,” Wong explained, adding there are concerns in the community about stigma.
ACO has been keeping a close eye on how Monkey Pox is progressing and we have invited Dr. Paul MacPherson to provide community partners and service workers with an educational zoom workshop and update on the status of Monkey Pox. <a href=”https://t.co/RO0d3WrFRN”>pic.twitter.com/RO0d3WrFRN</a>
—@ACOttawa
Brown was quick to point out that monkeypox is not a sexually transmitted disease, but that sex puts people in close contact. Those who are at high-risk should keep an eye out for symptoms and have any unusual rashes checked out by a health professional.
Right now, officials are taking a targeted approach to vaccination, said the virologist.
As for the rest of Ontarians, they can rely on lessons learned during the pandemic.
“We’re quite sensitive with COVID-19 still ongoing here,” said Brown. “Distancing and hand washing will go a long way to stopping the spread of monkeypox as well.”