OTTAWA —
With COVID-19 variants of concern continuing to spread across Canada, new national modelling shows that even the current level of public health measures will not be enough to prevent a resurgence of the virus nationwide.
The dire warning comes as part of the Public Health Agency of Canada’s (PHAC) new pandemic projections.
Looking at only non-variant COVID-19 spread, if Canadians maintain their current number of contacts the epidemic will continue to come under control. Factoring in the more contagious variants, the trajectory changes considerably and cases will spike again under Canadians’ current level of precautions and restrictions.
The presentation made by Chief Public Health Officer Dr. Theresa Tam and Deputy Chief Public Health Officer Dr. Howard Njoo notes that, with variants of concern now detected in all provinces with “increasing prevalence and spread,” if Canada wants to keep flattening the pandemic curve, more stringent public health measures and individual precautions are needed.
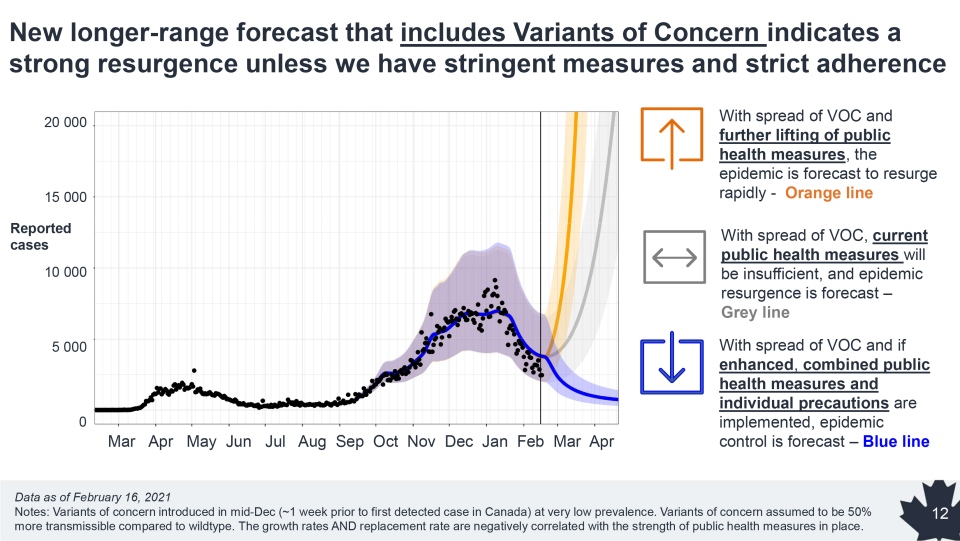
Based on the current projections, the current pandemic controls may not be enough to fully control the variants. The long-range forecast predicts a “strong resurgence” in March and April in all provinces.
Accordingly, if people let their guards down and if public health measures are lifted the variants are forecasted to send infection rates spiking to levels far past what was seen in either the first or second waves.
This could result in up to 20,000 new daily cases by the spring. Currently the average daily case count is approximately 2,900 new cases a day across the country, which is an improvement from last month when some provinces were reporting nearly that many new infections in a day.
On Thursday, Tam joined Prime Minister Justin Trudeau on the weekly call with the premiers. She was asked Friday if she’s raised her concerns about easing restrictions with her provincial counterparts, as some provinces have already started scaling back on their lockdown measures.
In response, Tam said they are aware that in her view a robust plan to sequence variants and contact trace needs to be in place before restrictions are loosened, and “if you ease anything at all, it better be slow with a lot of surveillance testing.”
She offered the recent surge in cases in Newfoundland and Labrador as an example of how rapidly new outbreaks of these variants can spread.
During a press conference on Friday, Trudeau said that while what provinces and cities have been doing is working, the threat of the variants remains.
“We have to keep taking strong public health measures… Otherwise we could see a third wave that is even worse than the second or the first,” he said.
Noting that this is not news anyone wants to hear, Trudeau said provinces looking to ease measures must be ready to respond to new outbreaks with swift action and suggested updates to the national COVID Alert app may play a role.
The modelling is focused on three variants of concern: the B.1.1.7 variant first identified in U.K. the B.1.351 variant first identified in South Africa, and P.1 the variant first identified in Brazil.
As of Feb. 18, PHAC data indicates that there have been 664 confirmed B.1.1.7 variant cases, 39 B.1.351 variant cases, and one case of the P.1 variant. Tam said it’s possible that, at least in the case of the U.K.-originating variant that it becomes a “very common” strain of the virus over time.
Based on the current pandemic situation, daily case counts, deaths and hospitalizations are currently declining in most of Canada and fewer health regions are reporting high rates of infection across all age groups.
The short-term forecast predicts Canada will see up to 878,850 total cases by Feb. 28 and total deaths could reach up to 22,420 people by the end of the month.
IMPACT OF VACCINES?
The modelling does not explicitly factor in the increasing rates of vaccination in Canada. However, it shows that international experience with these variants have been that while vaccine programs expand, stringent adherence to proper mask-wearing, physical distancing and other precautions have helped control the spread.
“For the next months we’re not going to have a lot of people vaccinated, that’s a fact,” Tam said. “In order for the vaccine to have the best runway it can to take off, you need to make sure those cases are kept low.”
Referencing these new figures during question period in the House of Commons, Conservative health critic Michelle Rempel Garner asked whether the modelling shows the federal government’s “failure” on vaccinations, and whether it’s “made Canada vulnerable to variants, and is going to create more lockdowns?”
In response, the parliamentary secretary to the health minister Darren Fisher said the federal government remains proud with more than 1.5 million vaccines delivered across Canada to-date.
Later, at the House of Commons Health Committee, MPs began hearing from senior PHAC officials about the current outbreaks, occurrences, and modelling for COVID-19 variant spread in Canada as it relates to projected vaccination rollout timelines, including the capacity to surveil, assumptions on vaccine effectiveness, and the procurement of booster shots.
During his testimony, Roman Szumski, the senior vice-president of the vaccine acquisition branch at PACH, said that Canada’s current vaccine contracts don’t talk about the need for potential boosters to deal with variants, so in order to access those, new contracts would be required.
“We are engaged directly with the suppliers and keeping current with their tracking of vaccine performance and plans for boosters or updates to their vaccines. They currently do not have boosters that are available,” he said.
In her remarks to the committee, Chair of the National Advisory Committee on Immunization (NACI), Dr. Caroline Quach-Thanh, said the variants are on NACI’s radar and many questions remain to be answered, though initial data around vaccine efficacy indicates the mRNA vaccines—which both Moderna and Pfizer shots are— show effectiveness against the U.K. strain, where as the others may pose more of a challenge.
“NACI is monitoring the data and will issue a statement if a booster or new dose is needed, including consideration of any new vaccine candidates that are authorized by Health Canada,” she said.