OTTAWA —
On Thursday, the Ontario government released data showing the percentage of COVID-19 outbreaks by location in Ottawa since August, following numerous requests for the data that led to the modified Stage 2 restrictions put in place on Oct. 10.
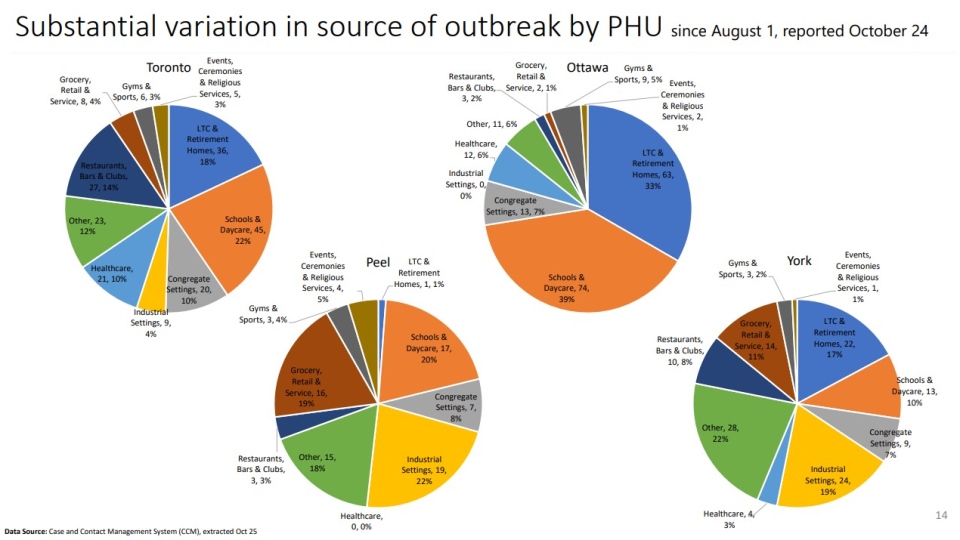
In Ottawa, long-term care homes, schools and daycares are responsible for the majority of COVID-19 outbreaks in Ottawa.
The data show schools and daycares account for 39 per cent of COVID-19 outbreaks in Ottawa since August 1, while long-term care homes are responsible for 33 per cent of the COVID-19 outbreaks. Restaurants and bars accounted for just two per cent of confirmed outbreaks in that time.
However, Ottawa’s medical officer of health has said that outbreaks are only one part of the picture.
Dr. Vera Etches noted that eight per cent of people who have tested positive for COVID-19 have said they had been to a bar or restaurant in the 14 days before their positive test result, meaning they may have contracted or possibly spread the virus at those locations.
Outbreaks accounted for about 24 per cent of all known COVID-19 cases in the past three months.
An “outbreak” is also a specifically defined event in public health terms. In long-term care or retirement home settings, a single positive case in a staff member or resident is enough for an outbreak to be declared, due to the higher risk of serious consequences in those settings. In childcare settings, a single symptomatic case in a child or staff member triggers an outbreak response. In schools, at least two cases must be confirmed and there must be evidence of spread within the school before an outbreak is officially declared. Two cases with a link between them are also required for a “community” outbreak in a workplace, such as bar or restaurant.
CTVNewsOttawa.ca looked at the data from outbreaks in Ottawa reported between Aug. 1 and Oct. 24 to break down the figures.
Schools and childcare
The figure that stood out in Thursday’s data about the number of outbreaks in Ottawa was the 39 per cent for schools and childcare settings.
Data from Ottawa Public Health show 78 outbreaks in schools and daycares between Aug. 1 and Oct. 24; however, these outbreaks have been consistently small, often ending with the minimum number of positive test results that triggered the public health response. There were also 14 outbreaks in childcare spaces before the first outbreak in a school was officially declared.
Of those outbreaks, 45 were in childcare spaces and 33 were in schools. These outbreaks accounted for 165 total cases (116 in children or students and 49 in staff) and zero deaths.
One childcare space had four cases in the time it was open; four childcare outbreaks led to three cases; five childcare outbreaks had two cases, and 32 had a single case. Data is missing from the spreadsheet provided by OPH in three outbreaks at childcare centres.
In schools, one outbreak led to 13 cases, while there were six additional outbreaks with five or more cases. Two outbreaks in schools led to four cases, four outbreaks in schools led to three cases, and 19 outbreaks reported just two cases.
Of all outbreaks in schools and childcare spaces that began between Aug. 1 and Oct. 24, 11 remain active as of Oct. 29.
Long-term care homes and retirement homes
There were fewer new outbreaks in retirement homes and long-term care homes in Ottawa than there were in schools and daycares, but the outcomes were much worse in the former than in the latter.
From Aug. 1 to Oct. 24, Ottawa Public Health reported 67 outbreaks in long-term care homes and retirement homes (31 long-term care homes and 36 retirement homes). These outbreaks led to 509 cases (277 in residents and 232 in staff) and 33 deaths.
It should be noted that, of these outbreaks, a single one at West End Villa is responsible for 127 total cases and 20 deaths.
Twenty-six outbreaks in long-term care and retirement homes began and ended with a single case. Two outbreaks with one case that began between Aug. 1 and Oct. 24 remain active. Twenty outbreaks involved five or more cases. Of those, 13 remain active as of Oct. 29.
Data is missing from two outbreaks in the spreadsheet provided by Ottawa Public Health.
Outcomes at long-term care homes and retirement homes have improved since the spring. While the number of COVID-19 outbreaks between March 20 and June 1 was much lower, at 35, they were far deadlier, accounting for 233 deaths out of 1,021 cases. This suggests staff at long-term care homes and retirement homes have become better at isolating and containing COVID-19 when it is detected in the home before it spreads.
Community outbreaks
Data on community outbreaks, such as in workplaces, sports and recreation, homes, and religious institutions, is much less clear.
Ottawa Public Health does not specifically identify the locations of outbreaks such as these, nor does it provide any information as to when the outbreaks began and ended, nor does it provide breakdowns of how many cases were linked to each individual outbreak.
Data from the Ontario government showed three outbreaks in bars and restaurants between Aug. 1 and Oct. 24, two in grocery and retail settings, nine in gyms and sports settings, and two in religious settings or events.
- Data from Ottawa Public Health show the following information for all community outbreaks:
- Religious/Spiritual Organizations: 1 closed outbreak, 6 cases, 0 deaths
- Residential: 1 closed outbreak, 14 cases, 0 deaths
- Sports and Recreation: 7 closed outbreaks, 54 cases, 0 deaths
- Workplace: 3 open outbreaks, 21 closed outbreaks, 158 cases, 1 death
According to OPH, there were 128 cases linked to community outbreaks between Aug. 1 and Oct. 24.
Community Transmission
Outbreaks accounted for 985 new lab-confirmed cases of COVID-19 in Ottawa between Aug. 1 and Oct. 24. There were 3,295 new cases in that same time period that are considered “sporadic” and were not connected to a declared outbreak.
The source of infection for all cases in that time varies, but close contact accounts for the majority of the known causes transmission in that time.
According to OPH data, 1,314 cases list close contact as the source of infection, while 963 people were exposed because of an outbreak.
However, there are more questions than answers for community transmission rates, as the source of infection is considered “missing” in 1,175 cases and is unknown in 638 cases, as of Oct. 29.
The data provided is a snapshot in time. The data can change as contact-tracing investigations reveal new information. This is especially true of cases reported within the last 14 days.
METHODOLOGY
Figures for this report were obtained via open source data provided by Ottawa Public Health.
Data for institutional outbreaks can be found here: https://www.arcgis.com/home/item.html?id=5b24f70482fe4cf1824331d89483d3d3
Data for community outbreaks can be found here: https://open.ottawa.ca/datasets/0df365456c254fbc942fe3d85c3dbf83
Data on sources of infection can be found here: https://www.arcgis.com/home/item.html?id=6bfe7832017546e5b30c5cc6a201091b
This report used data from Aug. 1 to Oct. 24, to match the information provided by the Ontario government on Thursday listing the number of outbreaks in Ottawa. The dates from the March to June comparison of long-term care and retirement home outbreaks included outbreaks that began between March 20 and May 27, 2020.