They say that timing is everything in life. That certainly applies to investing in the stock market, meeting your significant other, and deciding whether to wear clothes. But should it apply to when you get the bivalent Covid-19 vaccine booster? Should you worry about getting it too early or too late? Or should you just get it as soon as possible? Well, getting it now versus later is a good idea with three possible exceptions. Here’s why.
Getting the bivalent booster is indeed a bit like choosing whether to wear clothes. You don’t want to have any should’ves, could’ves, would’ves in the future. You don’t want to be saying, “perhaps I should have been wearing clothes when I ran into my boss in the elevator” or “what could have happened had I been wearing clothes while running into my potential soulmate in the museum?” Similarly, you don’t want to be lying in the hospital one day thinking, “yeah, probably should’ve gotten the booster earlier.” At the same time, it is unlikely that you will end up regretting doing either thing too soon. There may not have been too many times in your life when you have said, “If only I hadn’t been wearing clothes at the time.”
In a similar vein, let’s look at the current situation. It’s mid-October right now with November just over two weeks away. While you may be able to lose a guy in 10 days, it could take longer, at least two weeks, to get full immune protection from vaccination against Covid-19. Therefore, if you want to be protected as much as possible come November, it’s a good idea to get fully up-to-date on your vaccinations now.
And what might happen in November besides National Fun with Fondue Month? The answer rhymes with “a bro bid 19 merge.” For the past two years, November has seen Covid-19 surges. Take a look at the steep upward curves in the number of new reported Covid-19 cases each day that occurred in November 2020 and November 2021. Hmm, do you think it’s a coincidence that November is when the weather tends to get much colder and drier and activities typically move indoors? November is also traditionally a heavy travel month. Such conditions can really promote the transmission of the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2).
Upward swings in Covid-19 hospitalizations and cases have already been happening in Europe as I mentioned on September 26 for Forbes. Throw in the fact that many people in the U.S. and Europe have ditched Covid-19 precautions such as face mask wearing as if they were micro-sunglasses or cheetah-print slip skirts and conditions in general are ripe for yet another Covid-19 surge in the U.S. next month.
So, in the words of 2Unlimited, y’all ready for this potential next Covid-19 surge? Not exactly, if you haven’t gotten the bivalent booster yet. Unless you’ve recently had Covid-19, chances are your immune system is not that familiar with the most common circulating version of the SARS-CoV-2: the BA.5 Omicron subvariant. Over the past week, the BA.5 has constituted 67.9% of all Covid-19 samples reported to the Centers for Disease Control and Prevention (CDC). Previous Covid-19 vaccinations could offer at least some protection against the original SARS-CoV-2, the one that spread in early 2020. However, relying on just this protection can be sort of like your smartphone relying on an operating system from 2020 that hasn’t been updated since. Plus, your immune protection from Covid-19 vaccination may have waned and weakened over time. This could leave you vulnerable like a person without clothes this coming month.
According to CDC data, as of today, less than 5% of the U.S. population has gotten the bivalent boosters so far. That’s pretty darn low and leaves the U.S. vulnerable to what’s apparently happening in Munich, Germany, right now. As Peter Hotez, MD, PhD, Dean of the National School of Tropical Medicine, tweeted today, “if all eligible Americans get their new bivalent booster we might avoid” massive Covid-19 rises that end up overwhelming our not-so-difficult-to-overwhelm health care system:
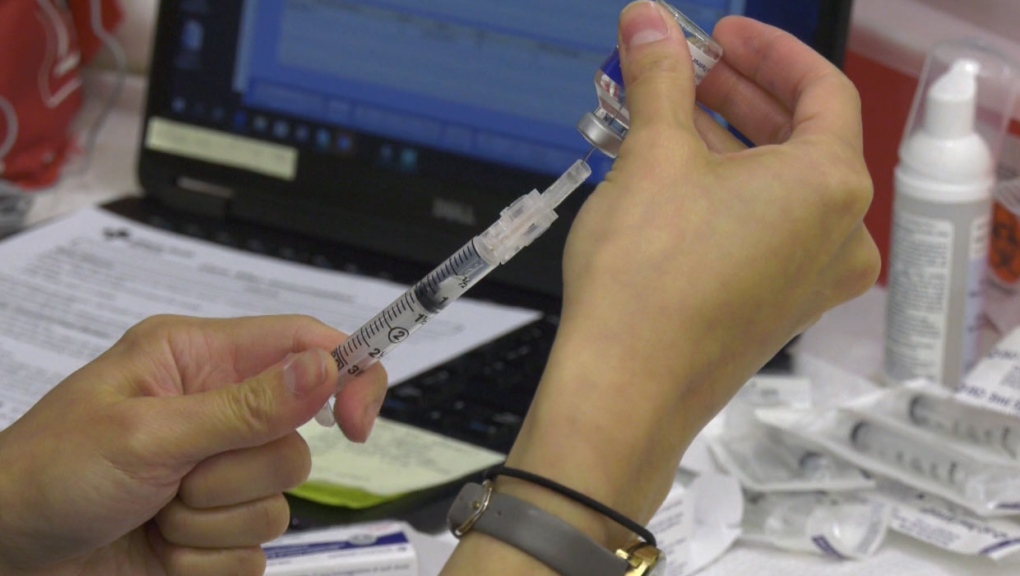
These new bivalent boosters are the first big update in the Covid-19 mRNA vaccines since, well, ever. As I described previously for Forbes, the Pfizer-BioNTech and Moderna bivalent booster vaccines are called bivalent because they contain messenger RNA (mRNA) for not just one type of spike proteins but two of them. These two types of mRNA will help your cells code for not only the original SARS-CoV-2 spike protein but also the spike proteins found on the surfaces of the BA.4 and BA.5 Omicron subvariants.
Could getting the bivalent booster right now be a bit too early? Today, a friend borrowed words from the song “My Shot” from the musical Hamilton when wondering whether getting the bivalent booster right now would be “throwin’ away your shot.” (By the way, that song from Hamilton was not about vaccination.) Sure, your immune protection may peak four to six weeks after vaccination and then start waning afterwards. Sure, that may leave you not quite as well protected January through March as compared to November and December. Nevertheless, waning immune protection is not like one of those warrantees on your tech devices where everything starts falling apart as soon as the warrantee expires. Instead, the waning should be gradual, meaning that getting vaccinated now should still leave you with a fair amount of protection for at least the next four to six months or so, as the World Health Organization (WHO) indicates.
White House COVID-19 Response Coordinator Dr. Ashish Jha speaks at the daily press briefing at the … [+]
Getty Images
If you are really worried about what may happen after six months, think about where you may be by then. It will be the Springtime when the weather should be warmer and more humid again with people moving activities back outside once more. That’s all assuming that a nuclear Armageddon hasn’t yet occurred, which certainly is always possible but may not be that likely. Meanwhile, no one can say for sure what variants and subvariants may be circulating by the Spring 2023. Chances are they will be different from the BA.4 and BA.5. So the real prime usefulness of the current bivalent boosters should be over the next six months.
On top of all that, our world could be in a very different situation come April and May. The Winter of 2022-2023 could potentially see the last one or two big Covid-19 surges before the pandemic is no longer considered to be a pandemic and instead has transitioned to a seasonal virus situation. So you might as well “hold on” in the words of Wilson Phillips and get up-to-date with your Covid-19 vaccinations now for what could be the Covid-19 pandemic’s last stand.
The three possible exceptions are if you’ve just gotten a previous version of the vaccine such as the older booster, just had Covid-19, or have been told by your medical doctor to hold off on getting vaccinated for some reason. The U.S. Food and Drug Administration (FDA) has indeed stipulated that before getting this new bivalent booster you should be at least two months out of previous Covid-19 vaccination such as getting the old booster. So if you are trying to get the bivalent too close to your last booster, the pharmacist may say, “bye Felicia” or “bye” whatever your name is and ask you to come back later.
If you’ve recently had Covid-19, the CDC is recommending that you wait at least three months before getting the bivalent booster, as I covered for Forbes on October 7. That’s because it may take your immune system a little while to recover from fighting Covid-19. And you want your immune system to be ready for the vaccine and ready to generate a proper full response. As I reported in that previous Forbes article, a study has suggested that waiting six months may give your immune system the full amount of time to recover from Covid-19, but it’s still unclear whether such a wait would necessarily be better.
Getting the bivalent booster alone will not offer 100% protection against Covid-19. As Winter … [+]
NurPhoto via Getty Images
So what do you do if you last got Covid-19 say in mid-June? It may seem like you are currently in the gray zone, being longer than three months out but not quite past the six-month mark. The challenge is that you can’t be sure what kind of immune protection you may have gotten from your last bout of Covid-19. It could be fairly strong. Or it could be relatively weak. Therefore, if you want to make sure that you are protected for a starting-in-November surge, it may be better to just get the bivalent booster right now.
Of course, there are situations where your doctor may tell you to wait for it, wait for it, wait to get your booster. For example, you may be getting some type of treatment that may be suppressing your immune system. Or you may be one of those rare individuals who has an actual ongoing medical reason not to get the vaccine. In any case, make sure that you are getting advice from a real medical doctor first. Your medical doctor should also give a clear scientific rationale for holding off on the Covid-19 vaccine. If the words “microchip”, “5G”, or “they’re coming to get you,” enter his or her explanation, you may want to find another doctor.
As a reminder, getting the bivalent booster alone won’t mean that you are completely protected from getting Covid-19. It won’t mean that you don’t have to maintain other Covid-19 precautions such as face mask wearing while in public indoors to avoid getting infected. That would be like assuming that wearing pants alone would be enough for a date or a job interview. Your interviewer or your date may say something like, “umm, where is your shirt?” As long as the pandemic continues, which certainly won’t be forever, consider vaccination to be only one layer of protection no matter when you time your vaccinatations.