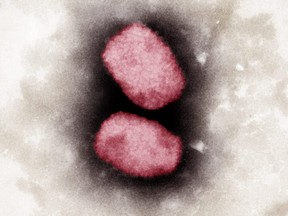
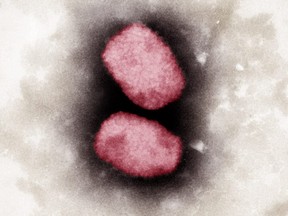
The World Health Organization has declared a public health emergency because of the global monkeypox outbreak,
Article content
Monkeypox vaccines will now be made available to high-risk groups, B.C.’s Ministry of Health announced Friday.
Advertisement 2
Article content
The ministry said that although the number of cases in B.C. remains low, some community transmission has been identified.
As of Wednesday, there were 61 cases of monkeypox in B.C., including three cases in Fraser Health, 54 in Vancouver Coastal Health and four in Island Health. There are no cases in Interior Health and Northern Health.
Health officials will be doing contact tracing for those who have been exposed to the pox.
The vaccine can be used as a preventative measure or given after exposure to prevent illness or severe outcomes.
It would be available to contacts of people who have monkeypox or people who are considered high-risk, said the ministry.
According to the B.C. Centre for Disease Control, the vaccine would be offered primarily to transgender people or men who have sex with other men and meet any of the following criteria:
Advertisement 3
Article content
• Have received a diagnosis of chlamydia, gonorrhea, and/or syphilis in the past two months, or
• Have had two or more sexual partners in the last 21 days, or
• Have attended bath houses, sex clubs, or park play, or plan to
• Have had anonymous sex in the past 21 days, or plan to, or
• Engage in sex work or plan to, either as a worker or a client
Health officials in B.C. say the monkeypox virus does not spread easily from person-to-person. All identified local transmission has involved prolonged skin-to-skin contact, which is suspected to be the primary way the virus is spread
To date, B.C. has received 14,480 doses of vaccine for outbreak control, including post-exposure prophylaxis.
Vaccines are ordered weekly and all doses are distributed to health authorities for administration. As of Wednesday, 7,200 doses were administrated to high-risk people, according to the health ministry.
Advertisement 4
Article content
Last week, the World Health Organization declared a public health emergency of international concern to manage the global monkeypox outbreak.
The Public Health Agency of Canada has urged gay and bisexual men to practise safe sex and limit their number of sexual partners to lower the risk of contracting the disease, which spreads primarily among men who have sex with men.
Monkeypox can occur in two stages, with flu-like symptoms appearing first, followed by a rash, usually with sores or blisters, though many people only get the rash.
The Centers for Disease Control and Prevention in the United States says 21,148 cases of monkeypox have been reported globally, with most of the cases identified in 71 countries, including Canada, that have not historically reported the illness.
— With files from The Canadian Press