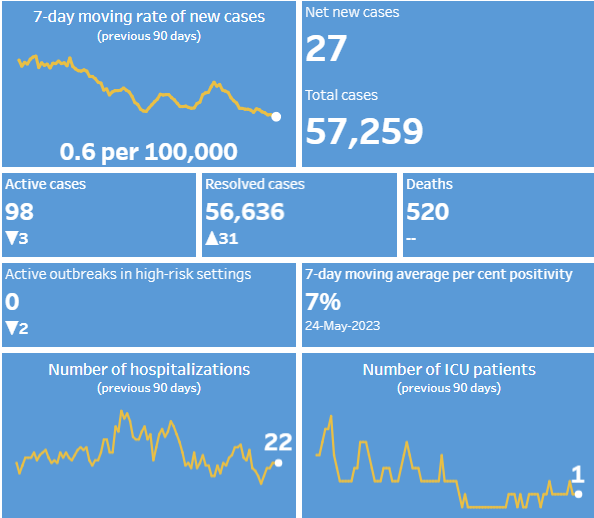
The Region of Waterloo is reporting no new COVID-19-related deaths this week, as well as zero active outbreaks in high-risk settings.
Outbreaks are recorded if found in long-term care or retirement homes, hospitals, or congregate settings – a category that includes shelters, group homes and correctional facilities.
Friday’s dashboard update shows the last two known outbreaks were declared over on Thursday.
Last week, the region reported its first COVID-19-related deaths in over a month after two people died.
The total number of COVID-19-related deaths in Waterloo region since the beginning of the pandemic remains at 520.
The number of people in ICU with COVID-19 remained consistent at one.

Meanwhile, the number of people in hospital with COVID-19 jumped to 22, an increase of five since last week.
The region has seen multiple updates in the last several weeks with no active ICU admissions.